By Dr. Ross Turchaninov, Phoenix
We thank everyone who commented on the original post. Those of you who mentioned Cauda Equina Syndrome were absolutely correct and we appreciate your clinical expertise.
The patient is 52 male who never had health issues before is owner of small windshield replacement company. As we mentioned in the original post he felt extreme electric shock pain in the right lower back and entire lower extremity after he lifted heavy windshield. Excruciating pain of high intensity brought him to his knees, caused complete drop of the right foot, sudden urination urge and he was almost immediately delivered into the emergency room.
This patient presented the worst-case scenario of disk problems. Instead of disk bulging or even herniation, the body of the L5 disk was sequestered and part of it slightly displaced to the right severely compressing L5 and S1 spinal nerves and creating a very complex clinical picture of Cauda Equina (a.k.a. Horsi Tail) Syndrome.
In these cases, besides severe lower back and lower extremity pain, the patients complain about abnormalities in the function of pelvic organs (delay or frequent urination, constipation, erectile dysfunction etc.). Another aspect of Cauda Equina Syndrome is the frequent presence of vasomotor abnormalities. It is the cause of the patient’s peripheral edema in the right leg and foot which was presented in the original post.
The presence of peripheral edema on the affected side means that compression of the spinal nerves is so severe that it blocks two-way traffic of the signals between CNS and tissues and organs. Compression and inflammation blocked the ascending sensory flow to the CNS and it triggered severe pain and dysfunctions which patient felt (pain, numbness, burning etc.). Same compression affected descending motor output from the CNS to the skeletal and smooth muscles and they lost normal tone.
Decrease of motor signals descending flow weakened skeletal muscles and it decreased the normal function of muscle pump responsible for the proper drainage. At the same time altered motor output weakened smooth muscles in the walls of veins as well causing their dilation. Failure of muscle pump in combination with veins dilation are two main mechanisms for this patient’s peripheral edema. The same impact on smooth muscle originally relaxed sphincter in urine bladder causing urination.
Cauda Equina Syndrome requires immediate surgical decompression due to the possible failure of the pelvic inner organs. The problem was that the patient did not have medical insurance and in emergency room he agreed on epidural injection only which brought him relief. While he was trying to figure out medical insurance issues, he came to our clinic to get some additional help.
Complexity and intensity of the clinical symptoms required gradual multi-disciplinary approach to his rehabilitation. While the patient continued to take his medications we extremely carefully started therapy with gentle application of Medical Massage protocol for Lumbalgia without provoking even slightest discomfort. Initially we concentrated on inhibitory regime of therapy to balance autonomic nervous system and suppress overactivity of pain analyzing system. Later on, we added more sophisticated modalities arranging them in the order to better use ‘lateral shift’ principle of Medical Massage. At the same time the patient started gentle exercises in the swimming pool and homework of passive stretching.
The Medical Massage protocol itself consisted of gradual addition of new modalities each time when the patient was ready for that and decompression of the soft tissues in the middle, lower back and sacral area on layer by layer basis (skin, superficial fascia, lumbar erectors, middle fascia, QL muscle, deep fascia, rotators and finally periosteum at the insertions into spinous processes, lower ribs, iliac crest, sacrum and SI joint). The local therapy on the foot and leg used same strategy but was added later when clear improvements of the symptoms and restoration of the function were observed. At the beginning locally we just maintained drainage using LDM.
During first 2 months (2-3 times per week sessions) the patient slowly, but steadily improved. At that point we were adding acupuncture, gentle manual therapy (without any adjustments) by DC, TENS unit along the sciatic nerve, passive stretching at home and recently very careful application of the inversion table.
We got so far that neurosurgeon who recently consulted the patient did not even consider the surgery anymore while continue to monitor his condition on the monthly basis. Peripheral edema started to dissipate first. Fig. 1 illustrates the patient’s feet before conservative decompression started and after 4 weeks of the therapy. Fig. 1 Illustrates the patient’s feet before the start of conservative decompression and after 6 weeks of therapy.
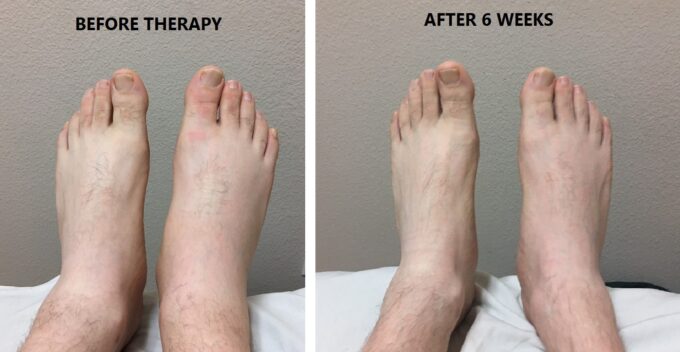
Fig. 1. Peripheral edema due to the vasomotor reaction before and after initial therapy.
Very light edema in the right foot is still visible as well as weakness of the big toe.
The patient entered our clinic still in pain and requiring support to move about. His right lower extremity was very swollen, and he continued to have to drag his right foot. Unfortunately, we don’t have a video of the patient at the beginning of therapy since it would have been unethical to ask for his permission at that time. The video below was recorded following 4 weeks of therapy after which the patient showed significant improvement and gladly gave us permission to record his improved but still abnormal gate. Notice that for the patient to walk steadily, he still needs to bend his right knee to elevate weak foot to refrain from stumbling. Peripheral edema in the entire right lower extremity is still visible. We repeated same short video 3 times.
The video below was recorded this week. The patient’s gate is normalized, and he is no longer bending his knee in an unnecessary way. The patient is able to maintain the transition of his foot from one stroke to the next. No visible and palpatory signs of peripheral edema. At this point, the patient shows only residual weakness in his right foot’s ability to support his gait.
Currently the patient doesn’t have any original symptoms besides residual weakness of foot extension and weaker toe elevation. Now he can lift all four toes on the right foot with the greater toe starting to jerk only this week, which is a great sign.
Successfully treated Cauda Equina Syndrome with the combination of somatic modalities, while Medical Massage was backbone of the therapy, one more time proves the exceptional clinical value of Medical Massage Therapy for patients even in dire situations.
As it was correctly pointed out in several comments to the original post that the patient was in a very difficult situation. His treatment must be approved and done in cooperation with the patient’s physician and the therapist must have very intense training and personal clinical experience. For many patients with Cauda Equina Syndrome the spinal surgery is only solution. However, if therapist has enough clinical expertise it is always worth it to try conservative therapy first.
LESSONS:
- You may see smaller peripheral edema in less severe cases of Sciatica. For Sciatica patients you have to test soft tissues for the hidden edema by applying mild compressions along the anterior foot and tibia. If even small depression stays in the tissue it is a sign of hidden edema and generally speaking you can’t expect very quick recovery since you are dealing with significant irritation/inflammation of the spinal/sciatic nerve. It takes time for the nerve to recover. Presence of any visceral symptoms which accompanied lower back pain (for example, constipation) is another red flag of severe or chronic spinal nerve irritation.
- The encouraging factor in this case was significant relief of symptoms’ intensity by the epidural injection. Usually it gives very limited help to patients with Cauda Equina Syndrome. Our theory of why conservative therapy worked is as follows: the disk was already compromised, but the brain was able to keep it in a compensatory state – he lifted heavy windshields from his truck – already compromised disk fragmented by the gravity and compression forces (at that point he entered decompensation state ) – first reaction of the brain to the alarm from damaged disk is protection – brain placed lumbar erectors, quadratus lumborum, iliopsoas and rotators muscle into the additional spasm to prevent any additional displacement of the disk – combination of fragmentation and excessive protective reaction triggered Cauda Equine Syndrome – epidural injection decreased initial protective reaction and the brain re-evaluated the situation and realized that despite of fragmentation being present there is no significant shift of the fragmented part of the disk – gradual elimination of protective muscle tension, restoration of normal mobility between layers of the soft tissues and decompression of the spinal segment by the therapy and water exercises eventually released pressure within the L5 segment and freed spinal nerve.
- At this point the patient has residuals of the initial nerve damage which we hope to fade away. If he continues his homework and stays away from lifting there is very good chance that fragmented part of the disk heals, but it is going to take time.
- It takes time for the injured nerve to recover and it also takes time for the therapy to work. Both therapist and patient must be patient. Sometimes for several sessions nothing happens, and it seemed that therapy reached a plateau. In reality, gradual and careful building up of clinical response paid off by suddenly giving another improvement.
- Accumulation of clinical expertise allows you to move from local therapy where the symptoms are (edema in this case) to identification and elimination of the actual cause. Otherwise be very careful with disk abnormalities, especially Cauda Equine Syndrome.
Category: Blog


