This article starts a three-part series on medical massage treatment and the rehabilitation of patients with Chronic Headaches (CH). We dedicate Part I to the origin and pathophysiological mechanisms, which are behind of the most common forms of CH practitioners encounter daily. In our clinic, we see many patients with CH, and we observe the striking clinical effectiveness of MEDICAL MASSAGE PROTOCOLs. From our own clinical observations and analysis of published scientific data, we are certain that correctly applied MEDICAL MASSAGE PROTOCOL is the first and, in many cases, the only treatment option for many patients with CH.
Application of massage therapy in cases of CH is widespread. Many patients found, on their own, that massage therapy is a very effective tool to decrease headache intensity. As a matter of fact, according to Gaul et al., (2011), 56.4% of patients with primary headaches use massage therapy as a treatment tool to control the intensity of headaches.
We regularly read and review articles in massage publications as well as on the Internet where various massage treatment options for CH are offered and discussed. Some of them offer valuable suggestions that practitioners should consider while others left us simply speechless. From inserting a finger into the patient’s mouth and compressing his or her hard palate for the treatment of Tension Headache to finger insertion into the ear canal to control Migraine, it seems that nothing stops some massage educators from coming up with absolutely wild and untested ideas that simply do not make even basic anatomical sense. Such publications convinced us to address the matter of CH and the clinical effectiveness of correctly designed MEDICAL MASSAGE PROTOCOL from a scientific point of view.
According to Stovner et al., (2007), 46% of the global adult population suffers from active headache. Hu et al., (1999) reported that migraine and migraine-type headaches have resulted in $13 billion in lost productivity and $1 billion in direct healthcare cost in the United States. These figures are huge, and massage practitioners who are able to offer a correct treatment protocol may build a successful practice based solely on CH treatment.
The major problem that current approaches to treatment of CH patients is that they only have management as a goal instead of finding and addressing the original cause to eliminate successfully CH. Of course, medical massage is unable to help all patients with CH but a significant number benefit from pain reduction without the use of strong analgesics, opiates or sedatives. In a great number of clinical cases, medical massage can completely eliminate CH and restore the patient’s health and productivity. We highly recommend readers carefully follow this three-part article to use the information we present to help patients with CH.
ORIGIN OF CH
There are many causes of CH and Migraine. Various medical sources propose different clinical classifications, and each has its weak and strong points. The frequently cited classification was proposed by the International Headache Society (2004).
The subject of Chronic Headache is extremely vast. Therefore, in this article, we will concentrate on Primary CH: Migraine (MG), Tension Type Headaches (TTH) and so-called Cluster Headaches (CLH).
MIGRAINE (MG)
MG patients are divided into two groups: Those who experience and those who do not experience aura. The International Headache Society (2004) defines the aura as a neurological symptom that usually precedes or accompanies the onset of headache. Usually, the patient experiences the same type of aura and starts to feel it at the same time before each headache incident. In the majority of cases, patients experience a visual aura, such as bright flashing lights (i.e., scintillation), partial vision decrease (i.e., scotoma), intolerance to light (i.e., photophobia). However, other types of auras may occur such as loss of smell (i.e., anosmia), decrease of skin sensitivity (i.e., hypoesthesia), etc.
Aura as a clinical phenomenon is thought to be related to a wave of spreading hyperexcitability and then depression over a particular area of cortical neurons. Those cortical areas that are affected the most alter sensory perception and produce symptoms of aura. For example, when hyperexcitability spreads through the visual cortex a visual aura develops. However, the majority of MG patients do not have aura while experience the same clinical symptoms of CH.
There are many theories offered to explain the nature of MG: neural theory, vascular theory, depolarization theory, neurotransmitter theory, etc. The most scientifically sound is the unified theory that combines the separate theories into a single, complex chain of events (Edmeads, 1991).
The vascular theory (Shevel, 2011) or the vascular part of the unified theory is especially valuable for massage practitioners. According to this theory, MG is a direct result of general vasoconstriction/vasodilatation of the small-innervated arteries that supply brain. The following is a proposed chain of events (see Fig. 1):
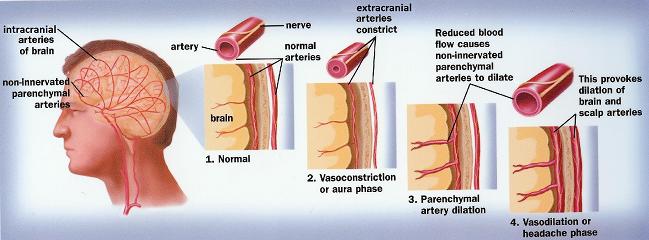
Here is general description of proposed chain of events:
1. The extracranial arteries, which supply scalp and periosteum of the skull and intracranial arteries located inside the skull and supply brain tissue, are linked via reflex pathways.
2. Tension in the posterior cervical muscles developed as a result of trauma and physical or emotional stress triggers vasoconstriction of extracranial arteries that supply the scalp. The vasoconstriction of extracranial arteries via reflex pathways triggers vasoconstriction of intracranial arteries that supply the brain. This vasoconstriction corresponds with the aura stage of MG.
3. As soon as the blood supply to the brain is even slightly compromised, the body will do whatever it takes to maintain normal blood perfusion through the brain. Thus, as a reflex reaction to vasoconstriction in the intracranial brain arteries, the parenchymal arteries (i.e., arteries that enter the brain tissue) dilate.
4. This dilation causes an exit of liquid into the surrounding brain tissue and even mild local swelling, which triggers an increase of the intracranial pressure. At this point, the MG attack begins.
As readers will see in the following articles, medical massage is unable to eliminate the clinical occurrences of MG with aura and MG without aura. However, medical massage may reduce intensity and frequency of attacks. Please also remember that patients who identify as having MG without an aura are very frequently misdiagnosed. The absences of reliable diagnostic methods create situations in which many patients with Tension-Type Headache (TTH) are wrongly diagnosed as experiencing MG. This frequent misdiagnosis is a disturbing trend since MEDICAL MASSAGE PROTOCOL has a dramatic and positive clinical impact on patients with TTH.
TENSION-TYPE HEADACHE (TTH)
The majority of patients with CH suffer from TTH, which is three times more frequent in the general population than MG (Stovner et al, 2007). Up to 78% of the general adult population will have TTH during their lifetime; approximately 30% are affected more than 14 days per year, and 3% are chronically affected (Jensen, 1999). Thus, practitioners see patients with TTH on a daily basis.
According to the International Headache Society (2004), “The exact mechanisms of TTH are not known.” However, various causes are being intensively studied. Extracranial muscle tension (Ad Hoc Committee, 1962; Lous and Olesen, 1982; Jensen et al., 1992) is the oldest of the discussed causes. Other potential triggers also reported include: increase of nitric oxide (Ashina et al., 2000); vascular abnormalities in cephalic arteries (Olesen, 1991); and central sensitization (Bendsten, 2000), etc.
However, for those who practice manual therapy and medical massage, one of the most intriguing causes of TTH is irritation or compression of occipital nerves. This is the main topic of our article that we discuss below.
CLUSTER HEADACHE (CLH)
CLH is form of MR or TTH where intense pain is concentrated around the eye. It is accompanied by excessive lacrimation, eyelid edema, forehead and face sweating, nasal drainage, restlessness, agitation and changes in vision. Usually one side of the head is affected.
The major problem for patients with CLH is the fact that for all these symptoms to happen the supraorbital and maxillary division of trigeminal nerve must be involved since these functions are in the domain of the 5th pair of cranial nerves (i.e., trigeminal nerve). We will address this issue below in greater detail.
OCCIPITAL NERVES NEURALGIA AS A MAJOR CAUSE OF MIGRAINE, TENSION-TYPE HEADACHE AND CLUSTER HEADACHE
ANATOMY OF THE OCCIPITAL NERVES
We suggest readers pay close attention to the information discussed below since it can have a positive impact on their patients and their practice. We will start with a short review of the anatomy of the greater and minor occipital nerves.
The greater occipital nerve (see Fig. 2) originates from the C2 spinal nerve and arises between the 1st and 2nd cervical vertebrae, bends under the belly of the oblique capitis inferior muscle, goes upward, pierces the semispinalis capitis and later trapezius muscle just below its insertion into the occipital ridge. The nerve appears under the scalp just above the occipital ridge, and runs under the scalp over the occipital and parietal parts of the skull giving local branches. The greater occipital nerve innervates the skin and scalp along the occipital and parietal pathways all the way to the anterior hairline.
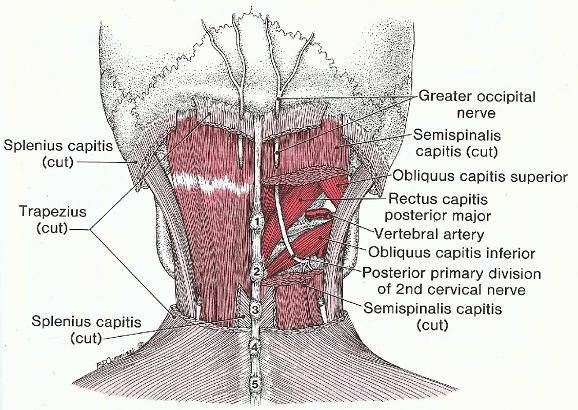
The lesser occipital nerve (see Fig. 3) also originates from C2, curves around and ascends along the posterior edge of sternocleidomastoideus muscle, just below the lateral part of the occipital ridge where it pierces the deep cervical fascia and continues upward under the scalp on the lateral side of the head to the temporal area. The lesser occipital nerve innervates the scalp and skin of the temporal area and outer ear.
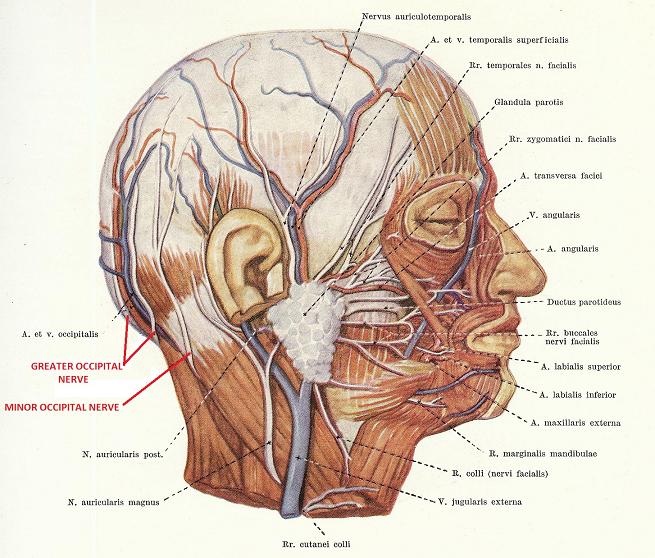
MECHANISM OF HEADACHE AS A RESULT OF OCCIPITAL NERVES NEURALGIA
In 1952, E. G. Edwards was among the first scientists to indicate Greater Occipital Nerve Neuralgia (GONN) as a possible origin of CH and MR. Since then, GONN as a major cause of CH has fallen in and out of favor among clinicians. Many other theories have been proposed since but recently more and more clinicians are again examining GONN and its role in the mechanism of CH and MG (Piovesan et al, 2001; Busch et al., 2004; Mosser et al., 2004; Bartsch, 2005). Let us discuss those findings.
As shown in Fig. 2 and Fig. 3, both occipital nerves have unusual anatomical pathways. In a great majority of cases, the peripheral nerves follow the easiest anatomical routes between muscles and other soft tissues. Very rarely do peripheral nerves actually perforate the tissue especially muscles. However, this is exactly what happens to both occipital nerves especially to the greater occipital nerve.
If one relaxes the posterior cervical muscles, the head falls forward because the anterior part of the head is heavier and the force of gravity and its weight pull the head forward. This is why the posterior cervical muscles work considerably in an isometric regime to fight the force of gravity by constantly pulling the head backward. The constant isometric work is one of the main reasons why the cervical muscles develop tension, spasm and active trigger points, which play a critical role in triggering TTH (Alonso-Blanco et al., 2011).
Active trigger points cause chronic extracranial pain that eventually hypersensitizes CNS and are directly responsible for transferring the episodic acute headache into chronic TTH (Bendtsen et al., 2011). It is a well-known fact that isometric contractions weaken blood flow in the working muscle by diminishing the effectiveness of the muscle pump, which plays a significant role in the oxygenation of the muscle during work.
As soon as even mild tension in the posterior cervical muscles is developed it causes mild irritation of the greater occipital nerve from a tensed trapezius, splenius capitis and/or oblique capitis inferior muscles (see Fig. 2). Even mild irritation of the greater occipital nerve causes sensory abnormalities in the areas of the head that are innervated by this nerve. The patient feels it in form of pain, tingling, burning sensation, etc. An ultrasound study conducted by Cho, et al., (2012) showed the cross section of the greater occipital nerve in patients with TTN and MG increases significantly when compared to the healthy subjects.
The more pressure on the nerve leads to a more diverse and intense headache experience by the patient. One of the great examples of the role tension in posterior cervical muscles plays in the development of TTH and MG is the so-called Orgasmic Headache, which is associated with acute muscle spasm triggered by sexual climax (Selekler et al., 2011).
In cases of severe compression of the greater occipital nerve by posterior cervical muscles, intense pain from the occipital area spreads throughout the entire half of the head all the way to the ipsilateral eye triggering CLH.
In cases of mild irritation of lesser occipital nerve in the area just below the lateral part of the occipital ridge, the patient will feel pain in the temporal area on the same side, which almost always mimics TMJ dysfunction. However, patients fail to complain to anyone about pain on the back of the head or behind the ear. We have seen many patients with a diagnosis of TMJ dysfunction who went through years of unsuccessful treatment including expensive night guards, injections, or manual treatments while the real cause was a mild irritation of the lesser occipital nerve.
Part II of this article will discuss diagnostic evaluation of patients with occipital nerve neuralgias. The practitioner must apply these simple tests to every new patient with temporal headache or the patient with an existing diagnosed case of TMJ dysfunction to eliminate Lesser Occipital Nerve Neuralgia. If pressure on the lesser occipital nerve is increased and the nerve is compressed, the patient will complain about pain originating in the occipital area especially behind the ear and radiating to the temporal area, ear and TMJ.
In addition to pain and other sensory abnormalities in the regions of the head innervated by greater or lesser occipital nerves, an equally important pathological outcome is vasoconstriction in the scalp arteries. As we discussed above in the section about pathogenesis of MG, the vasoconstriction of the scalp arteries is the first link in the chain of events responsible for the MG attack.
GOON AS A MAJOR CAUSE FOR CLUSTER HEADACHE (CLH)
The final important subject we would like to discuss in this article is the nature of CLH. There are many theories that try to explain the nature of CLH. Some of them view CLH as a separate type of headache while others see it more as a consequence of MG or TTH. However, all agree to the fact that to have CLH the patient’s trigeminal nerve must be involved and is difficult matter to resolve. The trigeminal nerve is cranial nerve that arises from the brain stem, to be precise, and passes inside the skull to appear on the face in three places: the ophthalmic, maxillary and mandibular (see Fig. 4). The trigeminal nerve is mostly a sensory nerve and provides sensory innervation of the face (i.e., touch, pressure, lacrimation, etc.) while the facial nerve is responsible for motor innervation (i.e., mimic musculature of the face). Trigeminal nerve also provides motor innervation of the masticatory muscles, tensor tympani in the middle ear and tensor veli palatine muscle which form soft palate.
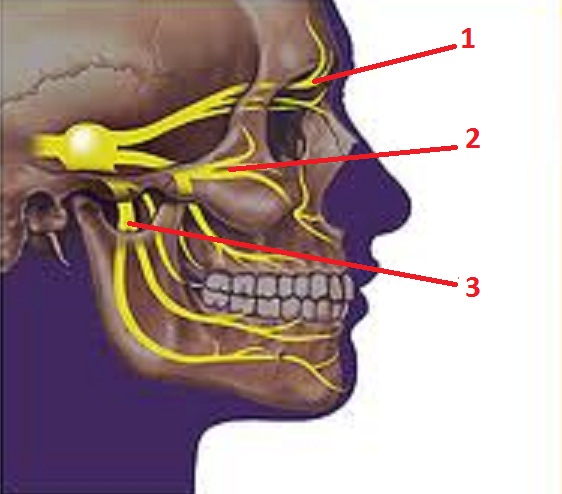
1 – ophthalmic division
2 – maxillary division
3 – mandibular division
For the CLH to develop, at least the ophthalmic division of trigeminal nerve must be involved, and in the clinical reality, both the maxillary and ophthalmic divisions are affected. There is no way that tension in the posterior cervical muscles can affect the trigeminal nerve because of its anatomical location inside the skull. Thus, one cannot attribute tension in the posterior cervical muscles as a reason for CLH. From another perspective, it is difficult to explain how patients who have MG with aura have CLH always on one side. For these patients the CLH has to be bi-lateral but clinically it is not the case. Thus, both scenarios (TTH and MG) do not exactly explain the mechanism of trigeminal nerve involvement and consequent CLH development.
Recently published papers found a very interesting correlation that perfectly explains the nature of CLH. The authors of these studies developed the concept of the trigeminocervical convergence (Piovesan et al, 2001; Busch et al., 2004; Bartsch, 2005). Electrophysiological experiments confirmed the existence of overlap between the pain analyzing systems within distribution of trigeminal and occipital nerves (especially greater occipital nerve). In such cases, this overlap serves as a relay between the peripheral (i.e. occipital nerves) and the central (trigeminal nerve) parts of CNS.
As studies show, the trigeminocervical convergence can be excitatory or inhibitory depending on the nature of stimuli the occipital nerves are exposed. For example, compressing the greater occipital nerve by posterior cervical muscles will excite the trigeminal nerve and trigger CLH. The inhibitory stimuli-for example, massage strokes (Piovesan et al, 2007), acupuncture (Granato et al. 2010), injection of local anesthetics combined with steroids (Young, 2010) or botulinum toxin (Selekler et al., 2008)-will block CLH by inhibiting activity of the trigeminal nerve.
This information is of great importance to practitioners because it theoretically justifies the already clinically known fact that massage therapy is a critically important tool to free the occipital nerves from pressure. The MEDICAL MASSAGE PROTOCOLs are how TTH and CLH can be completely controlled and the intensity of MG attacks diminished.
Part II of our article in the next issue of JMS, will discuss diagnostic evaluation of the patient with Chronic Headache.
Alonso-Blanco C, Fernandez-de-Las-Penas C, Fernandez-Mayoralas DM, de-la-Llave-Rincon AI, Pareja JA, Svensson P. “Prevalence and Anatomical Localization of Muscle Referred Pain from Active Trigger Points in Head and Neck Musculature in Adults and Children with Chronic Tension-Type Headache.” Pain Med. 2011. Oct.; 12(10):1453-1463
Ashina M, Bendtsen L, Jensen R, Olesen J. “Nitric oxide-induced headache in patients with chronic tension-type headache.” Brain. 2000. 23:1830-1837
Bartsch T. “Migraine and the neck: new insights from basic data.” Current Pain Headache Report. 2005. Jun.; 9(3):191-6
Bendtsen L. “Central sensitization in tension-type headache – possible pathophysiological mechanisms.” Cephalalgia. 2000. 20:486-508
Bendtsen L, Jensen R, Olesen J. “Decreased pain detection and tolerance thresholds in chronic tension-type headache.” Archives of Neurology. 1996. 53:373-376
Bendtsen L, Fernandez-de-la-Penas C. “The Role of Muscles in Tension-Type Headache.” Current Pain Headache Reports. 2011; Jul. 7
Busch V, Frese A, Bartsch T. “The trigemino-cervical complex. Integration of peripheral and central pain mechanisms in primary headache syndromes.”Schmerz. 2004. Oct.18 (5):404-10
Cho J.C., Haun D.W., Kettner N.W. “Sonographic evaluation of the greater occipital nerve in unilateral occipital neuralgia.” Journal of Ultrasound in Medicine. 2012. Jan. 31 (1):37-42
Edmeads, J. “What is migraine? Controversy and stalemate in migraine pathophysiology.” Journal of Neurology. 238(1):S2-S5, 1991
Edwards E.G. (1975). “The role of the greater occipital nerve in the production of headache.” JAMA. Ga. 1952. May. 41(5): 198-201
Gaul C, Schmidt T, Czaja E, Eismann R, Zierz S. “Attitudes towards complementary and alternative medicine in chronic pain syndromes: a questionnaire-based comparison between primary headache and low back pain.”BMC Complement Alternative Medicine. 2011. Oct. 7; 11:89.
Granato A., Grandi F.C., Stokelj D., Musho S., G. Pizzolato. “Acupuncture in Tension-Type Headache.” Neuroepidemiology. 2010. 35:160-162
Headache Classification Subcommittee of the International Headache Society. “The international classification of headache disorders, 2nd edition.” (ICHD-II) Cephalalgia. 2004. 24 (Suppl. 1):9-160.8
Hu XH, Markson LE, Lipton RB, Stewart WF, Berger ML. “Burden of migraine in the United States.” Archives of Internal Medicine. 1999. 159(8):813-818
Jensen R. “Pathophysiological mechanisms of tension-type headache: a review of epidemiological and experimental studies.” Cephalalgia, 1999. 19:602-21
Jensen R, Rasmussen BK, Pedersen B, Lous I, Olesen J. “Cephalic muscle tenderness and pressure pain threshold in a general population.” Pain. 1992; 48:197-203
Lous I, Olesen J. “Evaluation of pericranial tenderness and oral function in patients with common migraine, muscle contraction headache and combination headache.” Pain. 1982; 12:385-393
Mosser S.W., Guyuron B., Janis J.E., Rohrich R.J. “The anatomy of the greater occipital nerve: implications for the etiology of migraine headaches.” Plastic Reconstructive Surgery. 2004 Feb.; 113 (2):693-7; discussion 698-700.
Olesen J. “Clinical and pathophysiological observations in migraine and tension-type headache explained by integration of vascular, supraspinal and myofascial inputs.” Pain. 1991, 46:125-132.
Piovesan E. J., Di Stani F., Kowacs P.A., Mulinari R.A., Radunz V.H.;Utiumi M., Muranka E.B., Giublin M.L., Werneck L.C. “Massaging over the greater occipital nerve reduces the intensity of migraine attacks: evidence for inhibitory trigemino-cervical convergence mechanisms.” Arq. Neuro-Psiquiatr. Vol.65 No. 3a: Sao Paulo. Sept. 2007.
Piovesan E. J., Kowacs P.A, Tatsui C.E., Lange M.C., Ribas L.C., Werneck L.C. “Referred pain after painful stimulation of the greater occipital nerve in humans: evidence of convergence of cervical afferences on trigeminal nuclei.”Cephalalgia. 2001 Mar.; 21(2):107-9
Selekler M, Kutlu A, Dundar G. “Orgasmic headache responsive to greater occipital nerve blockage.” Headache. 2009 Jan.; 49(1):130-1
Shevel E. (2011). “The Extracranial Vascular Theory of Migraine – A Great Story Confirmed by the Facts.” Headache. 51 (3): 409-417
Stovner L, Hagen K, Jensen R, Katsarava Z, Lipton R, Scher A, Steiner T, Zwart JA. “The global burden of headache: a documentation of headache prevalence and disability worldwide.” Cephalalgia. 2007; 27(3):193-210
Selekler M, Kutlu A, Dundar G. “Botulinum toxin type-A (BOTOX) in the treatment of occipital neuralgia: a pilot study.” Headache. 2009 Jan.; 49(1):130-1
Young W.B. “Blocking the greater occipital nerve: utility in headache management.” Current Pain Headache Report. 2010. Oct.; 14(5):404-8
Category: Medical Massage
