The Editorial Board of JMS considers the publication of Prof. Melzack’s article as an important step in explaining to practitioners the scientifically sound data behind the origin and development of pain. The first and most important element of any successful somatic rehabilitation is control of the pain-analyzing system. Eventually, the practitioner will lose the battle against a pathological condition if the beast of the pain-analyzing system has not been tamed at the beginning. Thus, understanding how the pain-analyzing system works and application of correct somatic therapies are critical factors for every practitioner.
We were motivated to publish this article by the strange, unscientific and truly harmful misunderstanding of the modern science of pain evident among somatic practitioners. We have observed evidence of this misunderstanding on the Internet and, recently, in letters and comments sent to JMS.
Let us generally summarize the intentional or unintentional misunderstanding of the science of pain, which seems to be evident among somatic practitioners, including chiropractors, physical therapists and especially massage therapists. Here are the most common misconceptions we have observed:
1. Pain is generated by the brain as a protective response to perceived threat and it means that pain perception always has a central origin. Thus, the peripheral origin of pain is completely denied or is of far less importance than pain generated by the brain itself.
2. The peripheral origin of pain is an “outdated” concept that is not supported by modern achievements in pain science.
3. The role of pain receptors with their hyperirritability is minimized to the level of unimportance. Some practitioners even go as far as to state that: “There is no such thing as a pain receptor.”
4. In other words, a patient feels pain only in his or her head, since the brain is solely responsible for pain generation.
5. Based on these assumptions, treatment plans must be changed as well. Since there is no peripheral origin of pain or pain receptors, practitioners should work with patients to explain to them that their brain is the major reason for their pain, and previous experiences, such as suppressed emotions, must be addressed initially.
For those readers who think that we over-exaggerate the importance of this strange tendency, we have created a special page that can be accessed by clicking here. You will be able to read and judge actual posts from professional blogs and letters we have received that were written by a number of somatic practitioners from chiropractors and doctors of physical therapy to massage practitioners.
Practitioners who believe and spread these strange ideas claim they are based on the latest achievement of pain science: the Neuromatrix Theory of Pain (NT) developed by Prof. Melzack and Dr. Katz in 2012.
This and other articles on NT are widely cited to provide a scientific foundation to completely unscientific claims. At this point, large numbers of therapists strongly believe that NT has completely replaced the Gate Control Theory of Pain (GCT), which was developed in 1965 by Prof. Melzack and Prof. Wall.
In consideration of that, we need to take short trip into recent history. Before GCT was formalized, scientists had a very limited understanding of how the Pain-analyzing system worked. All theories in circulation at this time were different variations of an original pain theory proposed by the French philosopher Rene Descartes in the 17th century. This theory offered a very mechanistic approach to pain: i.e., pain is generated in the peripheral somatic and visceral structures carried to the brain through the nerves, and the brain develops the proper response.
GCT developed by Prof. Melzack and Prof. Wall changed this mechanistic approach to the issue, and transferred pain science from the periphery of medicine to main stream. Thus, GCT helped develop modern anesthesiology and pain medication. Somatic practitioners who assert GCT is an outdated science are, in actuality, relying on it every time they or members of their families undergo surgery or take pain medication. Thus, denying the existence of GCT is just an unbelievable hypocrisy.
We greatly admire Prof. Melzack’s work, and we are familiar with his and Dr. Katz’s article (http://onlinelibrary.wiley.com/doi/10.1002/wcs.1201/full). However, the conclusions of practitioners who have distorted the original ideas of NT are so biased that we were forced to analyze Prof. Melzack and Prof. Katz’s article and try to find any references to the strange views we observed and mentioned above. Of course, we did not find any justification for the existence and popularity of these misconceptions held by so many medical practitioners.
Our first intention was to publish a review article on this subject, which we thought would clarify this subject. An article published on the Internet in the form of a letter from Dr. E. G. Barton, MD expressed his strong opinion about such an “amateurish” approach to pain science (to review his letter please click here). Unfortunately, the response of the massage community was, let us say, gently, strange. One comment illustrated it well: “All these doctors don’t know much about pain.”
This type of response is why we decided to validate our data with the authors of NT. We are sure that their opinion will place everything in the correct perspective. We contacted Prof. Melzack who lives in Canada. We were thrilled that such legendary scientist, whose enormous contribution to modern science changed medicine, agreed to take the time to talk with us. Prof. Melzack was greatly surprised by the information we shared with him and the trends we have observed. He greatly sympathized with our viewpoint but since he has been fully retired from science for more than 12 years, he declined to be involved.
This is why we contacted Dr. Katz who was kind enough, despite his busy schedule, to grant JMS a short interview published in this issue. We think that Dr. Katz greatly clarified the major points of the NT theory and its umbilical relationship with GCT.
We see this current article as additional clarification of NT, and we will discuss this information based only on the reading of Prof. Melzack and Dr. Katz’s article.
Here are the false conclusions (emphasized in bold), and the correct reading of Prof. Melzack and Dr. Katz’s article on NT.
1. NT negates GCT
This issue is frequently mentioned. Dr. Katz addressed it in his interview but we would like to give an additional explanation. First, let us review what the article everyone has cited is saying:
“This (new data about phantom pain, by JMS) does not negate the gate theory (bold by JMS), of course. Peripheral and spinal processes are obviously an important part of pain, and we need to know more about the mechanisms of peripheral inflammation, spinal modulation, midbrain descending control, and so forth.”
The main problem with practitioners who believe that NT denies GCT lies in the fact they, in reality, are ignorant of the complete concept of GCT. From online posts we have read and letters we have received, it is obvious that these practitioners have never read the original article and think that GCT simply explains how pain is generated in pain receptors and channeled to the spinal cord and brain. The funny thing is that this description of the so-called pattern theories, which dominated the science of pain in 1950s, is exactly the theory that Prof. Melzack and Prof. Wall successfully put to rest in 1965 by publishing their classical article: “Pain Mechanisms: A New Theory” in Science.
The beauty and sophistication of GCT is that from the beginning, its authors emphasize the importance of the central mechanism of pain perception. Until 1965, no one else except Prof. Melzack and Prof. Wall thought about the central component of the Pain-analyzing system. The authors of GCT named it the Central Control Trigger. Let us quote Prof. Melzack’s and Prof Wall’s article published in Science (http://www.thera-bandacademy.com/elements/clients/docs/melzak1965__090707_160722.pdf):
“Thus it is possible for the central nervous system activities subserving attention, emotion and memories of prior experience to exert control over sensory input (i.e. pain stimuli, by JMS). We propose, therefore, that there exists in the central nervous system the mechanism, which we shall call the central control trigger that activates the particular, selective brain processes that exert control over sensory input.”
These are the exact words from the original article published in 1965, thirty-five years before the first article on NT was published. It is disappointing that anyone in the somatic rehabilitation field has the fortitude to even consider that NT invalidates GCT because the latter does not recognize role of the brain in pain perception.
To conclude this point, we would like to quote Prof. Melzack and Dr. Katz in this regard:
“The current status of pain research and therapy indicates that, despite the addition of a massive amount of detail, the conceptual components of the gate-control theory have stood the test of time (bold by JMS).”
Thus, opponents of GCT understood Prof. Melzack and Dr. Katz’s article in a distorted and amateurish way. NT has its origins in GCT, and they are connected by an umbilical cord. To deny GCT means that one denies NT and vice versa.
2. The peripheral origin of pain is an “old” concept that is not supported by NT. Pain is generated by the brain as a protective response to a perceived threat, which means that pain perception always has a central origin. Thus, the peripheral origin of pain is completely invalidated or it has much lesser value to pain generation by the brain.
NT is another step Prof. Melzack and Dr. Katz took to further explain the role of the brain in pain perception. The peripheral origin of pain is such a common and basic concept that denying that pain is triggered by pain receptors and even denying the existence of these receptors is like saying the Earth is flat. If we put everything in its correct perspective, GCT explains how pain originates and is conducted to the CNS, and the role the brain plays in pain perception. NT developed from there and, by using GCT as a foundation, further increased our understanding of the brain’s role in pain perception.
Let us again read the article for guidance. Fig. 1 is taken from Prof. Melzack and Dr. Katz’s article and graphically presents the basic concept of NT.
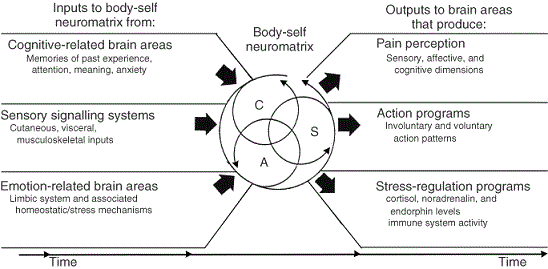
Please look on the left side of diagram. As somatic practitioners, the second component directly concerns us. As you may see, under the Sensory Signaling Systems, Prof. Melzack and Dr. Katz emphasized the importance of the somatic source of peripheral signals, which originated from various somatic and visceral structures and arrive at the brain to affect the neuromatrix. These are the areas where somatic abnormalities are developed, and it is therapist’s job to use medical massage and other means to eliminate them as soon as possible. However, some therapists who misunderstand NT are telling their patients that their pain is solely the product of their memories, emotions and previous life experiences instead of correctly and expeditiously treating the peripheral origin of pain.
Now look at the third component of the Sensory Signaling Systems. This is a significant justification of the importance of therapists who work in the stress-reduction field of massage therapy. NT emphasizes that stress greatly affects the emotion-related brain areas. Therapists can greatly reduce this sensory input to the brain and help maintain the health of their clients.
The middle part of the diagram indicates the body-self neuromatrix, which is the key component of the entire theory of NT. According to Prof. Melzack and Dr. Katz, the neuromatrix is a “network of neurons that consists of loops between the thalamus and cortex, as well as between the cortex and limbic system.” The neuromatrix of a newborn is determined by genetic factors but as the child develops, sensory input (including pain) additionally sculptures the neuromatrix.
The unique feature of the neuromatrix is the presence of these loops. These loops consist of many neurons that cyclically process to obtain and trigger sensory information on a constant basis. This simultaneous information-processing ability of the neuromatrix allows the brain to determine the best solution to respond to any sensory stimulation. In the diagram, these loops are represented by cyclical arrows.
The right side of the diagram illustrates the output of the neuromatrix. This output can be in different forms from the formation of pain perception to various voluntary and involuntary responses in the form of motor commands from the brain.
Thus, without properly delivered information from peripheral receptors including pain receptors, the neuromatrix will have a very limited ability to function properly.
As an example, let us look at how Prof. Melzack and Dr. Katz’s theory easily can be misread. This quote from the article is frequently used by proponents of the “only central origin of pain” as justification for their ideas:
“For example, when we respond to the experience of pain or itch, it is evident that the experience has been synthesized by the body-self neuromatrix (or relevant neuromodules) sufficiently for the neuromatrix to have imparted the neurosignature patterns that underlie the quality of experience, affect and meaning. Most behavior occurs only after inputs have been analyzed and synthesized sufficiently to produce meaningful experience.”
If one denies GCT and its unbreakable link to NT, the reading of this quote will justify that the neuromatrix or brain itself generates the sensations of pain and itch. However, the authors of NT describe what happens inside the brain after it receives any sensory stimulation, and how the brain processes the information obtained from the peripheral receptors. This is why those who distort NT never mention the points made by Prof. Melzack and Dr. Katz just two sentences below the one we have just quoted:
“When we respond to pain (by withdrawal or even by telephoning for an ambulance), we respond to an experience that has sensory qualities, affect and meaning as a dangerous (or potentially dangerous) event to the body. After inputs from the body (bold byJMS) undergo transformation in the body-neuromatrix, the appropriate action patterns are activated concurrently (or nearly so) with the neuromatrix for experience.”
As readers can see, the article emphasizes the importance of original sensory input from the peripheral parts of the nervous system as the first step in the chain of events that allows the “transformation (of sensory input from the body) in the body-neuromatrix.”
Thus, NT explains what happens in the brain and how it processes information after the peripheral part of the nervous system is triggered and any sensory stimuli (including pain) arrives at the CNS. Yes, Prof. Melzack and Dr. Katz in their NT specifically emphasize the fact that the brain itself is able to generate pain without any current activation of a peripheral component of the pain-analyzing system. However, even in this case, such activation is based on the previously received stimulation since its pattern is stored in the neuromatrix and it can be reactivated by memories, old emotions, etc. As readers can see, NT does not deny the peripheral origin of pain but clarifies and enforces its importance and gives us a better understanding of how sensory information, especially pain, is processed by the brain.
3. The role of pain receptors with their hyperirritability is minimized to the level of an unimportant issue. Some critics even go far enough to say that: “There is no such thing as a pain receptor.”
We do not even know how to respond to those who deny the existence of pain receptors or see them as irrelevant. Truthfully, how can one explain to a person who fanatically believes the Earth is flat that it is actually round?
Pain receptors were discovered in 1906 by English neurophysiologist Dr. Charles Scott Sherrington who coined the term nociceptors. In 1932, for this and other work on neurons, he received the Nobel Prize in Medicine. During the embryonic period, the nociceptors originate from neural crest stem cells, which later divide into nociceptors and mechanoreceptors. When the nociceptor matures, it is able to transfer any noxious stimuli (mechanical, thermal, chemical, etc.) into electrical impulses, which are called action potentials. Their summarized conductance to the spinal cord, and later to the brain, forms sensory input, which is the first step in pain perception (Fein, 2012). The phenomenon of the hyperirritability of pain receptors is a significant drop in the threshold of activation of pain receptors when they start to form and send action potentials to the CNS in the form of sensory ascending flow earlier than they are supposed even as a reactions to weak, unharmful stimuli. In a sense, the phenomenon of hyperirrability creates a condition of false alarms that are constantly bombarding the CNS, making it extremely responsive and sensitive to any pain stimuli originated in the peripheral receptors or in the neuromatrix itself.
Practitioners, including those who distort the science of pain, use this phenomenon on a daily basis obviously without realizing it. When the practitioner tries to find the location of active trigger point, he or she applies mild to moderate pressure to the skeletal muscle. The location of the trigger point is confirmed if the practitioner observes that the patient exhibits “Jump Symptoms” trying to withdraw the body from the examiner. This is living evidence of the phenomenon of hyperirritability of the pain receptors, which some somatic practitioners have eliminated from their assumptions of how the human body functions since these receptors do not fit into their distorted theoretical assumptions.
Of course, for somatic practitioners who live in their own bubble, this information is completely irrelevant. However, for those who have lost ground in this discussion, we would like to quote Dr. Woolf and Dr. Ma from the Department of Anesthesia and Critical Care at Harvard Medical School who generally describe the function of pain receptors or nociceptors:
“In order to deal effectively with danger, it is imperative to know about it. This is what nociceptors do–these primary sensory neurons are specialized to detect intense stimuli and represent, therefore, the first line of defense (bold by JMS) against any potentially threatening or damaging environmental inputs. By sensing noxious stimuli and contributing to the necessary reactions to avoid them–rapid withdrawal and the experience of an intensely unpleasant or painful sensation, nociceptors are essential for the maintenance of the body’s integrity. Although nociceptive pain is clearly an adaptive alarm system, persistent pain is maladaptive, essentially an ongoing false alarm (i,e. Phenomena of Hyperiirability, by JMS).”
4. Based on the incorrect reading of NT, the treatment plan must be changed as well. Since there is no peripheral origin of pain or even pain receptors, the practitioner should work with the patient to explain to them that their brain is the major reason for their pain and previous experiences and suppressed emotions must be addressed first of all.
The last part of Prof. Melzack and Dr. Katz’s article discusses the clinical outcomes of NT using examples of phantom limb pain, low-back pain and Fibromyalgia. Initially, it seems that the final part of the article supports the proponents of the incorrect interpretation of NT in their convictions. If the article gives clinical recommendations while the only central origin of the pain is present, it completely changes the clinical dynamic.
Of course, various continual education seminars are immediately offered to teach practitioners how to heal pain by using various somatic and psychological tools, and to convince the patient that it is not her median nerve that is compressed by transverse carpal ligament or his pain is not the result of spasms in the pifiromis muscle, etc. All these events have only one explanation: the patient’s brain itself is generating the pain perception based on bad memories or previous painful and emotional experiences.
Let us return to the article again and read it correctly once more. Yes, in the article the clinical application of NT is discussed. Yes, Prof. Melzack and Dr. Katz emphasize the importance of the central origin of pain as a structural component of treatment. The main idea of the article is that while working on the patient who is in pain, the practitioner must design a treatment protocol considering the peripheral and central origin of the pain. This is what the last part of the article discusses. In the section on low-back pain, the authors enumerate some therapies that are helpful and used for patients with lower-back pain: exercise, transcutaneous electrical nerve stimulation, ice massage, acupuncture, injections of anesthetics into the trigger points. All these therapies address the peripheral part of CNS to control low-back pain.
Prof. Melzack and Dr. Katz finished this section of the article with a sentence which leaves no doubt about their position and clinical recommendations:
“But no one therapy is more effective than the others. In fact, clinics often employ several procedures at the same time to get the best results.”
So how does NT affect the treatment protocol? The practitioner should divide patients into two major groups. The first group consists of patients who have developed somatic abnormalities as a result of direct trauma, chronic overload and irritation of peripheral nerves. For those patients, MEDICAL MASSAGE PROTOCOLs designed to deal with such pathological conditions are the first major treatment option.
The second, smaller, group consists of patients who exhibit a combination of chronic somatic abnormalities with simultaneous psychological changes. Some patients will reveal that to the practitioner at the beginning of treatment, some will hide it. However, the presence of such conditions is obvious. The client is depressed, nervous, easily agitated, easily gets emotional, etc. For those clients, the practitioner’s understanding of NT has far greater clinical value. For these patients, the first treatment option is not MEDICAL MASSAGE PROTOCOL but the reduction of stress with intense (speed wise) but gentle application of massage strokes especially various kneading techniques. As the degree of emotional and psychological stress continues to diminish, the sensory stimulation the practitioner evokes in the soft tissues is delivered to the CNS, which then re-arranges the activity of the neuromatrix. Only at this point, can MEDICAL MASSAGE PROTOCOLs be brought in.
We would like to once more emphasize to all our readers that successful somatic rehabilitation lies not in one theory or one modality used by the practitioner but in an integrative approach in which the practitioner has enough understanding to see the complete picture and determine the most efficient treatment protocol.
Melzack, R. Pain and the Neuromatrix in the Brain. J. of Dental Education, Vol. 65(12), 2001
Melzack, R., Katz J. Pain. Wiley Interdisciplinary Reviews: Cognitive Science, 4(1):1-15, Jan/Feb., 2013
Melzack, R., Wall, P. D. Pain Mechanisms: A New Theory. Science, 150(3699): 971-979, 1965
Sherrington C. The Integrative Action of the Nervous System. Oxford: Oxford University Press; 1906
Woolf,C.J., Ma Q. Nociceptors–noxious stimulus detectors. Neuron, 2007 Aug 2;55(3):353-64
Category: Medical Massage
