Ross Turchaninov, MD
In one day we had two patients with absolutely similar clinical symptoms. Those symptoms were numbness and burning pain in the left palm. The Sensory Test confirmed a significant decrease of sensitivity to touch on the left palm and Tinnel’s and Phalen’s Tests were positive in both patients. All of that indicated Carpal Tunnel Syndrome and that was exactly the diagnosis for both patients.
Both patients were unsuccessfully treated for Carpal Tunnel. However, the patients exhibited clinical differences which made their cases completely different. Patient #1 showed significant muscle atrophy of the left thenar muscles (see Fig. 1) and while Sensory Test on the left palm was positive it was negative on the left forearm
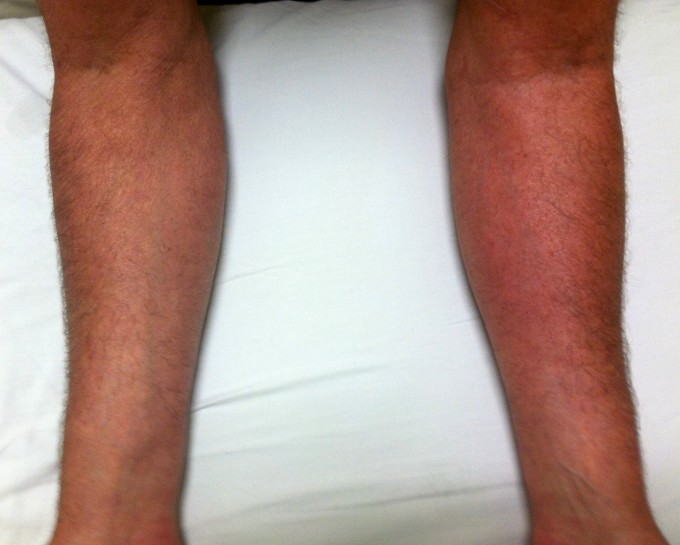
Fig. 1. Atrophy of thenar muscles in patient #1
Blue arrow indicates muscle atrophy in the thenar
Patient #2 didn’t show any atrophy, but his left forearm exhibited clear skin redness or local hyperemia (see Fig. 2) and the Sensory Test was positive on both surfaces of the left forearm.
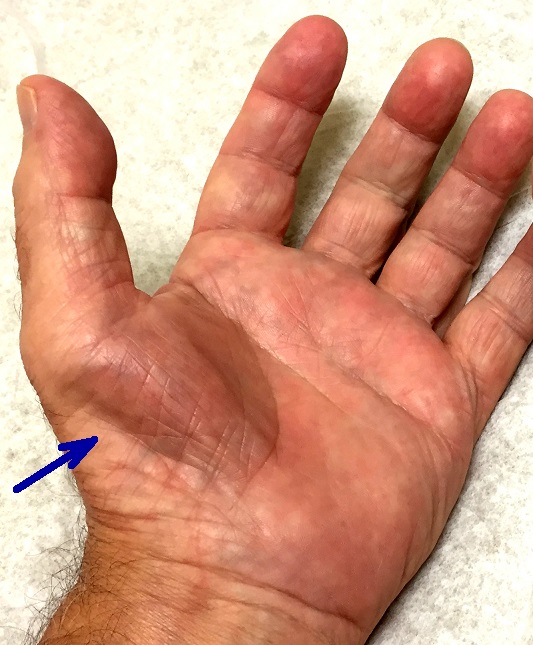
Fig. 2. Local hyperemia on the left forearm in patient #2
Notice the reddish color of the skin on the left forearm compared to the right one
In patient #2 there is no way pressure on the median nerve within Carpal Tunnel may trigger hyperemia of the forearm and a positive Sensory Test there, since carpal tunnel is anatomically lower, on the level of the wrist joint. In the case of this patient the only possible explanation was irritation of the brachial plexus or median nerve above the Carpal Tunnel.
Further evaluation of patient #2 showed that the Compression Test for Pronator Teres Muscle Syndrome on the anterior elbow was also positive, as well as the Compression Test for the Pectoralis Minor Syndrome on the front of the shoulder joint. However, the Compression Test (Wartenburg’s Test) for the anterior scalene muscle was negative.
So how do you interpret these findings? Patient #1 has 100% Carpal Tunnel Syndrome. Unfortunately, important time was lost and the median nerve now is irreversibly damaged. This is why the patient had such significant atrophy of the thenar muscles.
Patient #2 has symptoms like Carpal Tunnel Syndrome. The real cause was in the anterior shoulder where the pectoralis minor muscle slightly irritated part of the brachial plexus where the origin of the median nerve is. Since the Compression Test was positive on the level of anterior shoulder and application of the Compression test on the next upper level (anterior neck) didn’t trigger any symptoms down to the forearm and hand, the real cause of his symptoms on the hand was tension in the Pectoralis Minor Muscle.
Conclusion: Patient #1 must be treated by protocol designed to address tension in the Carpal Tunnel. However, the therapist must not say to the patient that treatment will completely remove the symptoms. Such extensive muscle atrophy the patient has means that the median nerve is severely damaged and there is no way its function will be completely restored. The patient at best may expect a decrease of intensity of uncomfortable symptoms.
Patient #2 must be treated with a protocol designed to reduce tension in the Pectoralis Minor Muscle since this is where the initial trigger is and after the brachial plexus is freed from the irritation, 1-2 sessions of the Carpal Tunnel Syndrome protocol should be used if needed.
LESSONS:
1. In every case of somatic pathology the mild to moderate irritation of the spinal or peripheral nerve, which supplies the affected area, must be ruled out first. Only if there are not symptoms of nerve irritation on the upper parts of the body should the treatment be local.
2. Patients with mild to moderate spinal or peripheral nerve irritation rarely complain about any uncomfortable sensations in the place of the initial irritation. Their symptoms will be located in the part(s) of the body where the irritated nerve ends. This fact is main cause of confusion among different health practitioners.
3. Never follow anyone else’s evaluation. Keep it in mind, but evaluate results presented you by the patient.
Category: Blog
