This Case of the Month was submitted by Dolores Champagne, CMMP, LMT who practices Medical Massage in Bristol, TN. From our perspective this submission is very interesting since it illustrates Dolores’ personal growth as a massage clinician.
Readers may observe her progress as a therapist while she worked on this complex clinical case. This is exactly what we are trying to trigger in our students – independent clinical thinking in combination with an individual approach to the treatment of each patient.
Ross Turchaninov, Editor in Chief
MEDICAL MASSAGE VS “UNSPECIFIED CONNECTIVE TISSUE DISORDER”
This case illustrates the clinical potential of Medical Massage, especially when it is applied correctly. I took my first Medical Massage seminar with the Science Of Massage Institute in April of 2014. I was hooked! I knew this was the training I wanted to pursue, the kind of massage I would like to practice from now on and these are results I wanted to deliver to my patients. During my next Medical Massage seminar in October, 2015 I mentioned to Dr. Ross Turchaninov the patient I had with an “Unspecified Connected Tissue Disorder.” He informed me that with this disorder, full resolution of her problem would not be possible but that I could greatly improve quality of her life.
This case is very important to me because it opened the door to a full blown Medical Massage practice which I continue to successfully build up.
This case started with a 41 year-old female who came to my office seeking treatment for Plantar Fasciitis. Her secondary complaints were Chronic Headaches and pain in the neck and both shoulders. She also had pain in her major joints due to Osteoarthritis, high blood pressure and Type 2 Diabetes. She was also diagnosed with Peripheral Neuropathy on her legs and feet. Her chronic pain was identified as the result of “Unspecified Connective Tissue Disorder.” She was taking eight medications. She worked as a nurse in an allergy clinic. The patient used therapeutic massage regularly, but it brought her only minor relief for 2-3 days.
TREATMENT
1st session (March 2016)
The evaluation and treatment session took me an hour and 35 minutes. During her clinical interview I discovered that she had bilateral calcaneal spurs, technically not Plantar Fasciitis. Here is the X-ray of the foot where the large calcaneal spur (marked with red arrow) and ossification at the insertion of Achilles tendon to the calcaneus (marked by blue arrow) are clearly visible. Two black lines indicate shadow of Achilles tendon.
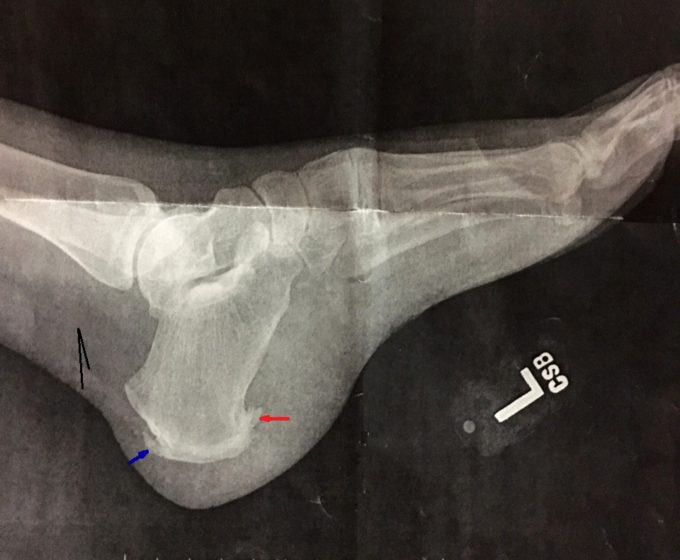
I used MEDICAL MASSAGE PROTOCOLs for Calcaneal Spur Syndrome and Cervicocranialgia. The patient returned in 2 weeks reporting some improvement in her feet and significant improvement in her neck and shoulders.
2nd session
A small light bulb came on. I included Myofascial Release holds and Connective Tissue Massage on her lower legs and feet. I also continued with Cervicocranialgia and Calcaneal Spur Syndrome Protocols.
After the second session her improvement had lasted 7-10 days, so I suggested we try weekly sessions to try to establish a “new normal.”
At this point I obviously did not understand how to go about obtaining stable clinical results. Although I had read in Medical Massage, Volume I textbook about timing of treatment sessions, it had not sunk into my brain what I actually needed to do.
3rd session
Treatment time 1:20 and I feel that I am too slow or I am trying to do too much in one session as the patient had 1 hour sessions scheduled.
4th-8th Sessions
For the next 6 weeks of regular weekly sessions I mixed Myofascial Release and Connective Tissue Massage while incorporating them into MEDICAL MASSAGE PROTOCOLs. Finally my patient reported that she could not remember the last time she had a headache and her “restless legs” were not keeping her up at night.
In another 2 weeks she reported that the intensity of neuropathy symptoms in her feet was down to a 3 without medication!
In following sessions I added MEDICAL MASSAGE PROTOCOL for Achyllodynia. It was obvious that her “Unspecified Connective Tissue Disorder” was mostly responsible for her symptoms down to the legs and feet. To address these symptoms I used Tissue Displacement Techniques (e.g., Scrolling Kneading), on her legs in order to take pressure from the deep fascia. This therapy in combination with CTM to address superficial fascia gave the best results to my patient.
CURRENT RESULTS
As it is right now the patient has been completely off neuropathy medication for the past two months. On a bad day her pain level is at 5 whereas before it was a 9 – 10 with medication. The patient used to take Ambien to help her with sleep. Her last Ambien prescription was filled in March. The most she takes for pain now is ibuprofen and that is not daily.
Her headaches have lessened from 2 to 3 per week down to 1 or 2 a month, mostly related to allergies or high stress days.
The client has noted significant improvement in the function of her immune system. She correlated this effect with the application of Medical Massage and the effect it may have on her lymphatic system. She doesn’t get sick as much, but when she does it is not as severe as it had been in the past.
She still has symptoms of Osteoarthritis in the lower joints, but the intensity of
symptoms is much less in the hip joints and mostly affecting her knee and ankle joints.
From now on my treatment priorities will change since I will switch to the application of MEDICAL MASSAGE PROTOCOLS for Osteoarthritis in knee and ankle joints.
My patient credits Medical Massage for great improvements in her symptoms and restoration of her quality of life.
In spring of 2014 I was working at a spa doing therapeutic massage as well as a few years in a
clinical setting at a chiropractic office. I was frustrated with my clients coming in every two
weeks to get an adjustment and a massage and always having the same complaint. They never
seemed to get any better although they felt better when they left.
I began searching for something that would improve my skills. I came across the Science of
Massage Institute. It was exactly what I was looking for and that first seminar just blew me away. It was so much useful information and much more then I bargained for.
So here I am, just over two years from when I started, five weekends, countless hours on my “soft parts” as Dr. Ross would say and I now have my own growing practice in medical massage. I am so excited to be on the forefront of change in the massage world. I knew there had to be something more and I found it with SOMI.
Category: Case Studies
Tags: Issue #4 2016

