This clinical case sent to JMS by one of our former students, Allen Stanley, LMT, CMMP, CMLDT strongly illustrates the value of Medical Massage Concept. Most of the Medical Massage (MM) sources incorrectly represent MM as an independent clinical modality. However, modern medicine sees MM as flexible and inclusive of different techniques and modalities previously tested in the clinical practice. Thus, a Medical Massage practitioner is a therapist who has enough clinical knowledge and expertise to read the patient’s body and to create individually designed treatment protocols using different treatment options offered by MM.
Allen exhibited a deep understanding of MM because he could correctly prioritize and use MM techniques to step-by-step address post-surgical edema, restricted mobility of soft tissues, and the scarification of grafted skin. His efforts greatly paid off by returning pain-free functionality to his patient.
Dr. Ross Turchaninov, Editor in Chief
MANUAL REHABILITATION OF BURN PATIENTS
by Allen Stanley, LMT, CMMP, CMLDT
The patient is a 42-year old female who works as the owner and operator of a trucking business. In early August of 2021, the patient suffered second and third-degree burns from spilled boiling water on her lower legs and feet. The burn trauma was so severe that she was transported to a burn center in Gainesville, Florida, where she had multiple surgeries and skin grafting mostly on the right leg and both feet.
Before the accident, I worked on this patient to decrease tension and multiple adhesions in her fascia and other connective tissue structures developed after several C-sections. Thus, the fascia which covered her lower extremities was already affected due to deep scars and adhesions formed on her lower abdomen.
EVALUATION
Clinical Interview
I saw patient for the first time at the beginning of October when her doctor gave permission for further rehabilitation of soft tissues. The patient could hardly walk into the clinic due to the pain and tension in the upper thighs, legs and feet. In her thighs the significant tension was in the areas of Rectus femoris, Vastus Lateralis, and Vastus Intermedius. In these areas the skin was harvested for grafting.
However, the most painful areas were the lower legs and feet, where grafting was done. Aside from severe pain, tension, and numbness, the patient couldn’t tolerate anything touching her feet, even bedsheets. This indicated that the patient suffered from a severe case of causalgia (extreme skin hypersensitivity due to hyperirritability of peripheral receptors) as an indicator of reflex zones formed in the skin.
Visual Evaluation
A visual evaluation of the patient’s skin indicated insufficient venous drainage on both feet and legs but with right affected the most. The soft tissues exhibited glossy skin reflecting light due to the peripheral edema, skin pigmentation and peeling. Signs of peripheral edema were also registered along the posterior aspect of L5 dermatome and the anterior aspect of L2-L3 dermatomes.
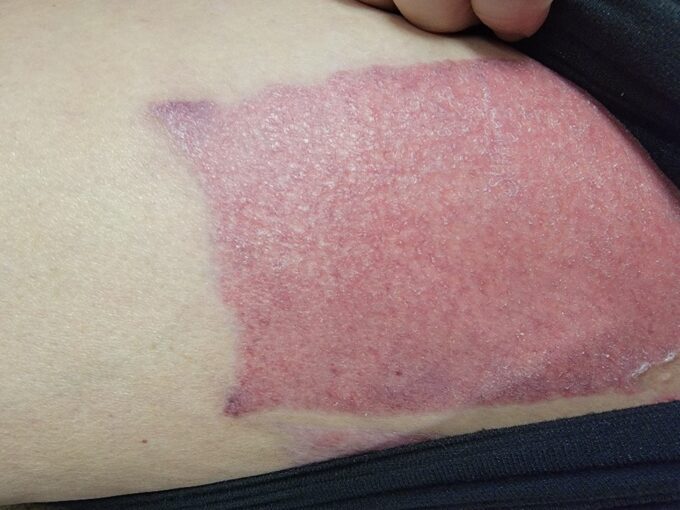
On anterior and medial surfaces of both thighs areas of skin harvesting indicted with red, swollen areas (see Fig. 1).
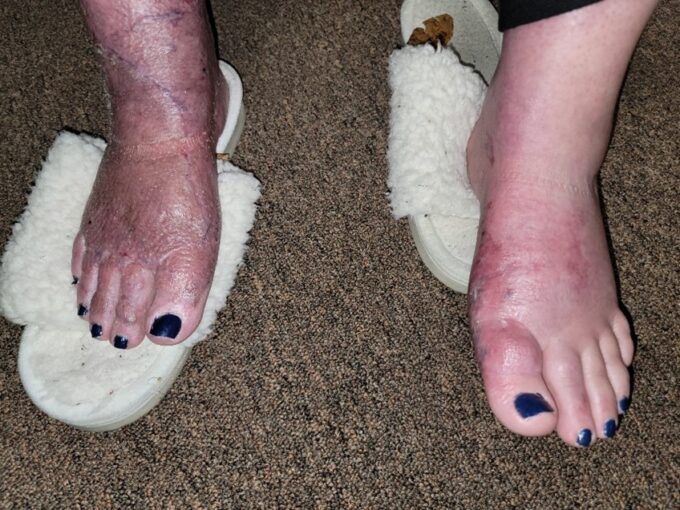
Fig. 2 demonstrate the clinical picture at the evaluation session
Palpatory Evaluation
A Sensory Test (decrease of skin sensitivity) was positive along the affected dermatomes (L2-L3 and L5). A Compression Test indicated pitted edema on both feet and legs up to the knee-level.
A palpatory examination of the skin harvesting areas in the thigh and grafted skin in both feet and legs confirmed significant skin tightness and decrease of the skin’s elasticity. It was impossible to examine the skin’s mobility since skin couldn’t be moved under any pressure applied laterally to shift it. Forming and lifting a fold of skin could only be done above the unaffected tissues. Peripheral edema and skin tightness in the feet can be seen in Fig. 2.
Another piece of the evaluation puzzle was the slightly edematous soft tissues in the middle and lower back. Mild edema spread to the posterior thighs and was confirmed by positive Sensory Tests.
Therefore, the evaluation confirmed severe adhesions formed in the areas of skin’s harvesting and skin grafting which, in combination with the initial trauma, greatly affected drainage. It created a vicious cycle as the fluid retention triggered the formation of new adhesions and the hardening of preexisting ones that contributed to further drainage failure.
The peripheral edema compressed the cutaneous nerves triggering sensory abnormalities in the form of tingling and numbness.
Finally, fluid retention in the traumatized tissues overwhelmed the lymphatic system forming secondary milder edema in the upper parts of the body up to the middle back.
TREATMENT
The main goals of my therapy were to:
1. Control the edema and restore proper drainage from all compromised areas.
2. Restore elasticity and proper function of the grafted tissues.
3. Normalize skin’s innervation.
The patient couldn’t lay on her stomach, so I started her face up in a supine position. I started with MLD on the head and cervical lymph nodes to open up the lymphatic system and worked my way down to her thoracic areas, draining upper watersheds along the anterior-axillo-anastomosis (AAA) and the axillo-inguinal anastomosis (AI). I used Vodder’s Technique combined with proper breathing, starting with a normal rate and slowly increasing it times ten. It is an excellent tool to assist lymph movement and enhance MLD.
I incorporated work on her legs and feet during the following sessions using MLD. I added small half-circle strokes with a series of nine repetitions starting from thighs to feet. The tissues responded very well to this therapy by decreasing the edema and gradually increasing the grafts’ elasticity. MLD triggered Lymphangiomotoricity in the soft tissues. The fluid movement from the affected tissues was easy to observe since the structure of soft tissues changed while MLD was done. Every time I finished working on her legs and feet, I drained a new lymph, which entered the system further up to the Axillary areas and Thoracic Duct.
During the final part of the session, I addressed adhesions and scarification of the grafted skin. I first used Microcurrent MPS and then engaged grafts in Scar Therapy to increase the mobility of the grafted skin and decrease adhesions formed between grafts and underlying soft tissues. With short push/stretch strokes I learned in SOMI classes, I began to displace the grafted skin in the direction of the most prominent tension. I added the same applications across lines of tension and then tried to form a fold of skin and eventually rolled the fold of grafted skin to restore the skin’s fluidity against the fascia, superficial skeletal muscles and periosteum.
From session to session, the patient became more mobile, her ROM gradually increased, and she was able to lay on her side and finally on her back which immensely helped the entire MLD protocol.
Fig. 3 indicates an intial and current current clinical picture of our patient.
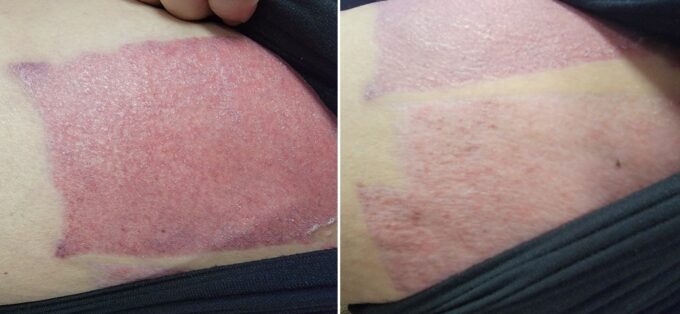
Fig. 4. presents an initial and current clinical picture of the patient thighs where the skin was harvested. You may notice partially restored skin color and a decrease in peripheral edema (the skin exhibits normal skin tension). The patient was able to return to her trucking business fully.
BIO
My name is Allen T. “Tim” Stanley. I’m from Florida and have lived in WV for many years. I first studied massage back in WV and renewed my studies in Florida with an excellent instructor named Jeff Woods after recovering from a stroke in 2015-2017. While studying massage therapy, he introduced me to the Science of Massage Institute (SOMI) and the work of Dr. Ross Turchaninov.
Microcurrent Point Stimulation helped me heal after my stroke and several neck fusions. I began studying it in 2013 and later add MPS for scar therapy and to decrease adhesions and increase connective tissue elasticity. Recently I got my Manual Lymphatic Drainage Certification in Pre-Post Surgery, which helped me feel fully equipped to treat others.
Now I combine SOMI’s education in Medical Massage with other somatic modalities. This comprehensive approach has significantly increased my patients’ healing time frame. I continue to pursue my clinical education working with SOMI and my mentor Dr. Ross. My MM clinic, “Keep Young Massage LLC,” is in Lady Lake, FL. I live in Clermont, FL, with my wife Sharon, who keeps me on track to help others with their medical problems.
Category: Case Studies
Tags: 2021 Issue #3