By Dr Ross Turchaninov, Phoenix, AZ
This is the final segment of our article on extremely efficient treatment options for Periosteal Massage.
Here are links to Parts I-IV:
Let’s discuss the step-by-step implementation of Periosteal Massage (PM). First, PM is not an independently applied modality but rather the final part of comprehensive somatic rehabilitation of the affected area. In other words, PM is used at the end of the Medical Massage Protocol after layer-by-layer decompression of the soft tissues has been completed.
As discussed in the previous parts of this article, the cause of periosteal dysfunction is tension in the soft tissues inserted into the periosteum and its direct trauma. Without detailed work to eliminate the tension in the soft tissues, the PM will not deliver stable clinical results in re-attaching the periosteum to the bone.
Now, let’s review the PM application. As we mentioned in Part IV, the primary repair force in the human body is fibroblasts, which are activated by trauma and inflammation in tissues and organs. Histamine released by affected tissues is the main driving force in the awakening and movement of fibroblasts to the injured or inflamed site (Groeger et al., 2020).
When periosteal dysfunction and trauma form, the locally present fibroblasts attempt to repair the periosteum and restore function. They produce pro-collagen, uploaded into the inflamed periosteum so mature, fully-functioning collage fibers can re-attach the periosteum to the bone. However, since the trauma and inflammation in cases of periosteal trigger points are very local and sometimes even pinpointed, there are too few engaged fibroblasts. Thus, regular muscle contractions quickly destroy the deposited pro-collagen because the patient needs to type on the computer, drive the kids to school, carry groceries, etc. Thus, everyday activities don’t assist in proper healing.
Therefore, we need a larger number of fibroblasts working at the injured site to upload enough pro-collagen so that even though some of it will be destroyed, a sufficient amount remains to mature into normal and fully functioning collagen fibers. In other words, local periosteal dysfunction results from repairing labor force shortage. There is no other clinical solution until the issue of fibroblast recruitment is solved. This is precisely what PM does!
Let’s consider that the patient suffers from Lateral Epicondylitis, a.k.a. Tennis Elbow. After decompressing soft tissue within the dorsal forearm layer-by-layer, the therapist addresses the site of periosteal dysfunction. As mentioned above, PM is conducted ONLY in the areas where the inflamed bone is covered by skin only. A therapist tries to damage the periosteum in this area by applying cross-friction and powerful compressions well above the patient’s pain threshold.
Generally speaking, the therapist who practices clinical aspects of MT must work below or ON the patient’s pain threshold level in correctly conducted treatment. Any therapy that exceeds this threshold ruins the treatment due to the brain’s protective reactions. However, in periosteal dysfunction, the soft tissue is present in only two forms: skin and periosteum. Thus, the patient’s brain-protective reactions are minimal.
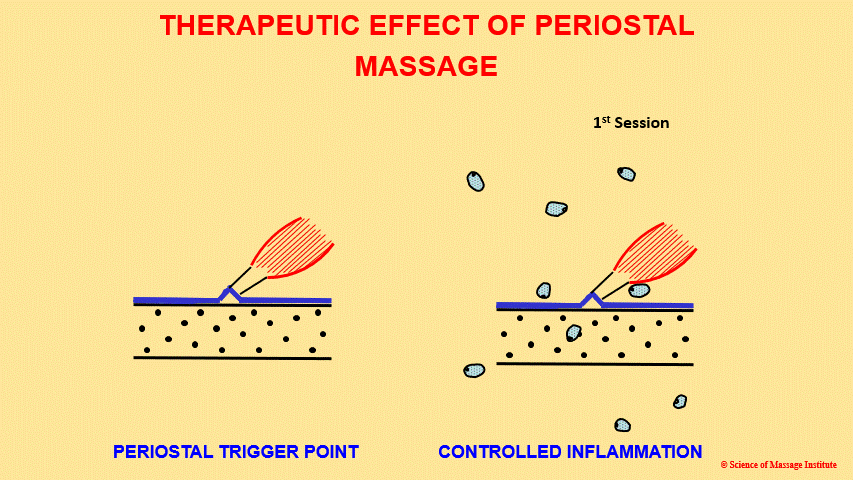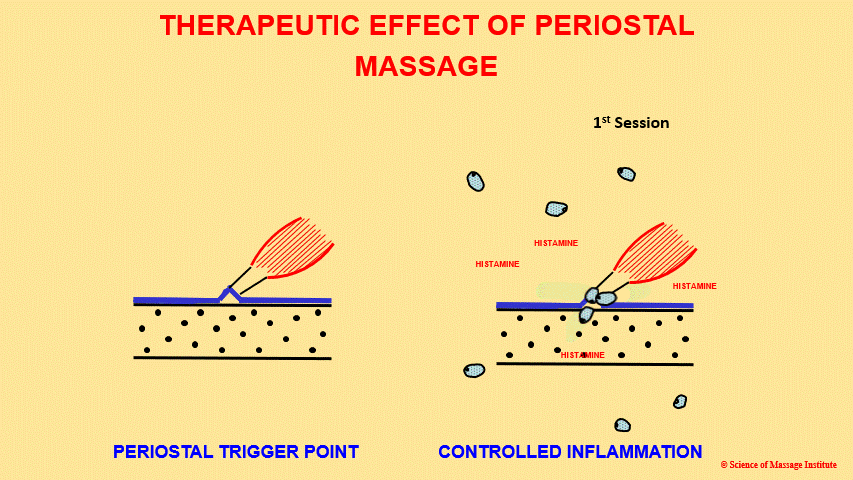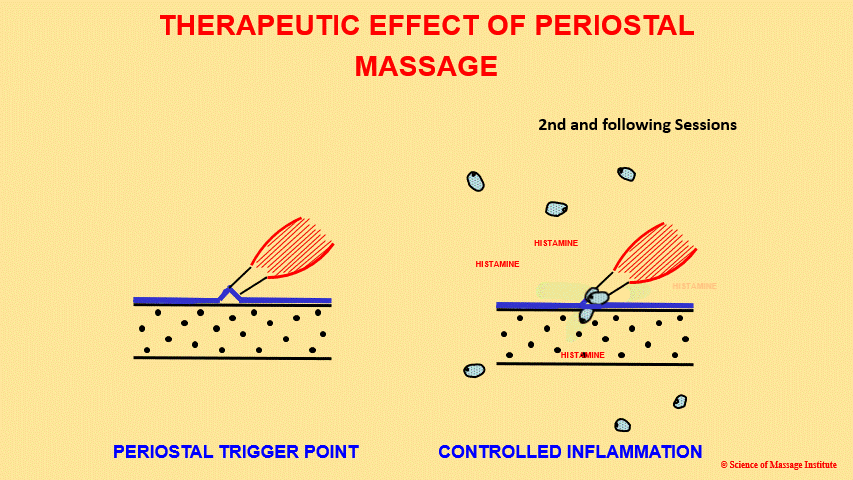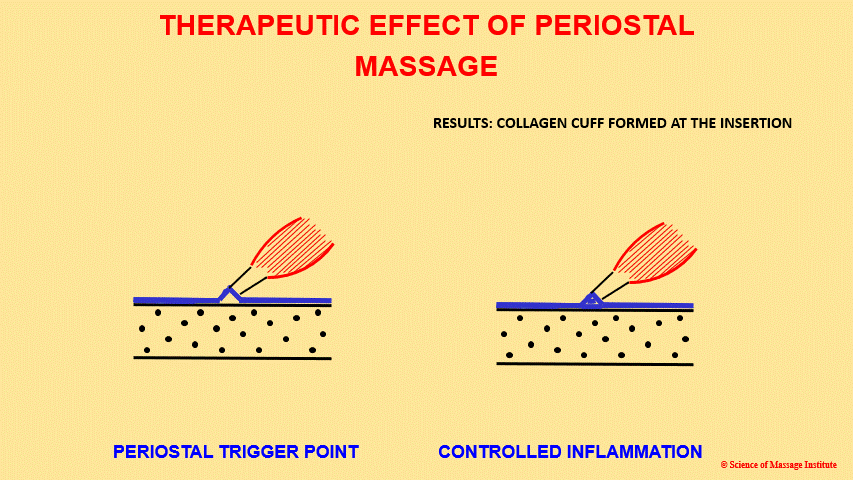
It is reasonable to ask: The periosteum is already inflamed and traumatized in the affected area of periosteal dysfunction. In such a case, why do we need to additionally traumatize the periosteum? To answer this question, we will use interactive Diagram 1. For the animation diagram to play and re-play, please double-click in the middle of the diagram.
Let us describe that diagram. On the left, changes in the patient’s elbow in cases of Tennis Elbow are schematically presented. You see the bone of the lateral epicondyle (two black lines with black dots between), the periosteum detached from the bone (blue line) by the tendon, and the muscle belly of the extensor digitorum (black and red lines). Blue pieces that appear during PM application indicate new collagen deposits in the place of injury and inflammation.
When a therapist traumatizes the periosteum, they trigger so-called controlled inflammation, which increases the local concentration of histamine at the site of periosteal dysfunction. As a result, additional fibroblasts are activated, and pro-collagen is produced and uploaded (the first movement of fibroblasts in the diagram). Two to three days after the first session, the initial flare-up reaction starts to fade away, and that is when the next session needs to be implemented. The decreased intensity of the flare-up reaction means that the local concentration of histamine in the place of periosteal dysfunction has dropped, and a new porting of histamine needs to be generated in the area of periosteal dysfunction.
The therapist re-traumatizes the inflamed periosteum again, and, as a result, the histamine level rises. The body sees this as a sign of a larger trauma requiring extra assistance. Fibroblasts from neighboring areas, which were not even massaged, start to converge at the site of periosteal dysfunction, greatly increasing the number of fibroblasts and the amount of pro-collagen deposited into the periosteum.
We want the reader to pause to appreciate the following paragraph fully. While doing PM, the therapist completely controls the most critical cellular healing force in the human body – fibroblasts! The therapist decides to continue the employment of the fibroblasts or, if they are no longer needed, let them go back to inactive dormancy in the form of fibrocytes.
As a result, PM creates so-called collagen cuffs (Haine, 1997), which additionally reinforce tissue. The exact mechanism of fibroblast attraction and their activation contributes to wound healing (Cao et al., 2103).
TECHNICAL APPLICATION
The techniques of PM are very simple. The therapist uses intense cross-fiber friction and compression at the insertion of a tendon or ligament into the periosteum well above the patient’s pain threshold. It is very uncomfortable during the therapy and can be extremely painful the next morning. The first treatment session when PM is used must be scheduled before a patient’s day off.
After the first PM session, the pain can be intense, with all the classical signs of local inflammation. However, even during the second session, the practitioner and patient will notice a significant difference in the intensity of the discomfort during and after the treatment. It will diminish with each session until the periosteal reflex zones are eliminated (Yankovsky, 1982).
The therapist should see the patient on the day that the sensation of pain and discomfort in the area of PM application starts to fade. It is usually two or three days after the first session. The following sessions can be scheduled on alternate days.
There are three possible scenarios for Tennis Elbow or similar disorders:
1. The patient only has an active periosteal trigger point (i.e., Periostitis).
2. The patient has local Tendinitis only.
3. The patient has a periosteal trigger point or Periostitis AND Tendinitis.
There are some differences in application. If the patient has only Periostitis, the therapist may use as much pressure as the patient can take. If the patient has Tendinitis, the intensity of the strokes must be diminished to the pressure just slightly above the patient’s pain threshold. In these cases, the therapist IS NOT using PM but rather Cyriax’s Therapy or cross-fiber frictions (Cyrax, 1985). Finally, for the combination of Peristitis AND Tendinitis, the therapist must use different degrees of pressure and two treatment options: PM in the areas of Periostitis AND Cyriax’s Cross fiber friction in the area of Tendinitis.
Usually, the site of a periosteal trigger point and inflamed tendon are very close to each other. The video below illustrates the location of an inflamed tendon where milder pressure in the form of Cyrax’s friction should be applied and the tip of the lateral epicondyle where full application of PM should be used.
Before using both PM and Cyra’x Friction, the therapist MUST stabilize the skin by stretching it between two fingers of the other hand. The video below illustrates skin stabilization when applying cross-fiber frictions and PM.
There is a way to dramatically decrease the intensity of discomfort after the first couple of sessions and generally speed up the patient’s recovery. In patients’ best interest is getting a local steroid injection from their primary care doctor or orthopedic doctor three or four days BEFORE the therapy starts (Troisier, 1991). We use this approach when working with patients with Periostitis and Tendinitis. If the patient doesn’t want a steroid injection, they must be advised about the possibility of severe initial reactions.
Finally, any antihistamine medication (anti-allergy or antacid) must be discontinued two or three days before starting treatment. Histamine’s antagonism prevents the migration of fibroblasts (Groeger et al., 2020) and defeats the purpose of treatment.
SCIENTIFIC AND CLINICAL SUPPORTING DATA
As we mentioned above, the original idea of periosteal dysfunction as a result of direct trauma or reflex zones formation, as well as PM as a treatment method, was developed by two German physicians, Vogler and Krauss (1953).
From the beginning, these authors emphasized that periosteal dysfunction can result from trauma and overload of soft tissue and reflex zone formation in the periosteum due to its inappropriate innervation (Diekmeier, 1963).
Troisier (1991) compared the clinical effectiveness of cortisol injections (257 cases) to the application of cross-fiber friction (131 cases). According to the results, the cortisol injection fully relieved pain in all cases, but 66.7% of the patients had a reoccurrence within one to three months. 83% of the patients were completely healed in the group treated by PM. The author concluded that combining cortisol injection and massage is the most effective clinical approach to treating Tennis Elbow.
Based on detailed clinical studies of PM, Vogler and Krauss (1953) concluded that the local vasomotor reflex in the soft tissues, called axon-reflex, is a major contributing factor in the local therapeutic effect of PM. However, scientists from Indiana University Health Ball Memorial Hospital were able to reconstruct the entire mechanism behind the healing power of cross-fiber friction and PM in a series of laboratory experiments on rats (Davidson et al., 1997; Gehlsen et al., 1999).
After triggering Tendinitis in the Achilles Tendon in rats by repetitively injecting an enzyme called collagenase, the authors applied intense cross-fiber friction on the tendon and at its insertion to the heel bone. The scientists used light, electron, immuno-electron, and gait analysis to examine their results. They registered up to 375(!) newly arrived fibroblasts on average, compared to 190 registered in the control group, where cross-fiber friction with very light pressure was performed. Additionally, all fibroblasts in the experimental group exhibited a highly developed rough endoplasmic reticulum, which was clear evidence of the stimulation of pro-collagen production within the cells.
Thus, the authors experimentally proved the claims of many clinicians that the repetitive application of mechanical stimuli and generating controlled inflammation in the already traumatized and inflamed soft tissue would attract, activate, and stimulate fibroblast activity.
REFERENCES
1. Cao TV, Hicks MR, Standley PR. (2013). “In vitro biomechanical strain regulation of fibroblast wound healing.” Journal of Osteopathic Medicine. Nov. 113(11):806-18.
2. Cyrax, J. Theory and Practice of Massage. Textbook of Orthopaedic Medicine, Vol. 2. 11th Edi-
tion, Bailliere & Tindall, Toronto, 1985.
3. Davidson, C.J., Ganion, L.R., Gehlsen, G.M., Verhoestra, B., Roepke, J.E., Sevier, T.I. (1997). “Rat Tendon Morphologic and Functional Changes Resulting from Soft Tissue Mobilization.” Medicine & Science in Sports & Exercise Journal, 29: 313-319.
4. Diekmeier L (1963). Periosteal Reflex Zone Massage: Diagnosis and Therapy. Hippokrates Dec.15;34:940-4
5. Gehlsen, G.M., Ganion, L.R., Helllfst, R. (1999). “Fibroblast Responses to Variation in Soft Tissue Mobilization Pressure.” Medicine & Science in Sports & Exercise Journal. 31(4): 531-535.
6. Groeger M, Spanier G, Wolf M, Deschner J, Proff P, Schröder A, Kirschneck C. (2020). “Stimulatory effects of histamine on the migration of nasal fibroblasts.” PLOS One. Aug. 7;15(8):0237040.
7. Haine, H. (1997). Lehbruh der Biologischen Medicine. Stuttgart, Hippokrates.
8. Krauss H. (1953). “Clinical and experimental contributions to Vogler’s periosteal treatment.” Archives of Physiotherapy (Leipiz).; Schriftenreihe 2:51-168.
9. Troisier, O. (1991). “Tennis Elbow.” Rev. Prat., 41(18):1651-1655,
10. Vogler, P. and Krauss, H. (1953) Periostbehandlung. Leipzig.
11. Yankovsky, G.A. (1979). Osteoception, Zinatie, Riga.
ABOUT THE AUTHOR
Dr. Turchaninov graduated with honors from the Odessa Medical School in Ukraine in 1982. He was admitted to the residency program of the Kiev Scientific Institute of Orthopedy and Rehabilitation, which he completed in 1985.
He worked as a supervisor of the rehabilitation program for the Ukrainian Ministry of Public Health. During these years, he also worked with the medical team of the relief effort following the Chornobyl nuclear plant disaster. Later on, Dr. Turchaninov worked as a senior scientific researcher at the Kiev Scientific Institute of Orthopedy and Rehabilitation.
In 1989, Dr. Turchaninov obtained his Ph.D. degree in medicine, and in 1990, graduated from the Kiev Scientific Institute of Orthopedy and Rehabilitation’s manual therapy and medical massage programs designed for physicians.
In 1992, Dr. Turchaninov was invited to work in rehabilitation centers in New York City and Scottsdale, Arizona, as head of their medical massage program.
Dr. Turchaninov is the author of more than 100 scientific papers and publications in both European and American medical journals. He is the author of three major textbooks: Medical Massage, Volumes I and II, and Therapeutic Massage: A Scientific Approach. He lectures in the U.S. and abroad on issues of manual therapy and medical massage and is regularly invited to speak at American and international conferences.
Dr. Turchaninov is the founder of the Science of Massage Institute dedicated to bringing clinical science into massage therapy and educating therapists on the clinical applications of Medical Massage. He is the Editor in Chief of the Journal of Massage Science.
Category: Medical Massage
Tags: 2023 Issue #2