This clinical case was contributed to JMS by a recent graduate of SOMI’s Medical Massage Certification Program, Kristi Tidwell, LMT, CMMP from Coolidge, AZ. Her experience is interesting from two perspectives. First, it illustrates the clinical value of Medical Massage as the cornerstone of somatic rehabilitation. For years, a long list of various modalities was used that failed her patient; only Medical Massage decisively eliminated HER pain and dysfunction.
The second aspect of this submission is how masterfully Kristi combined components of different Medical Massage protocols, constantly adjusting the structure of each treatment session. By doing that, Kristi carefully and steadily built up an effective clinical response, restoring normal elasticity and functions of the soft tissues while resetting the patient’s sensory and motor cortex.
Dr. Ross Turchaninov, Editor-in-chief
MEDICAL MASSAGE vs. FRUITLESS PAIN MANAGEMENT
By Kristi Tidwell, LMT, CMMP
Coolidge, AZ
The patient is a 62-year-old retired female. Her symptoms appeared several decades ago with right side lower back and hip tightness and discomfort. Initially, symptoms started as a tightening across the top of the right gluteal area and later transformed into pain, which spread down along her lateral thigh.
Symptoms progressively worsened, and in late 2018, she started to feel severe left hip pain to the degree that she couldn’t walk to the mailbox. By then the pain had become burning, especially along both lateral thighs. Any extra physical activity, such as bicycling, increased pain and discomfort. The intensity of the bilateral hip pain progressed to such a degree that she could only walk about 800 steps and then had to stop and rest for 10-15 seconds before being able to continue walking.
Since the first symptoms developed, the patient went through many different therapies, none of which provided stable clinical results:
- Trigger point injections along the entire length of her lower back and outer thighs, totaling 32 in 2019
- Cortisone shots in the trochanteric bursa, two in 2019 and in April 2023
- Spinal manipulations
- Spinal decompression treatment
- Physical therapy treatment
- Regular Massage Therapy
- Foam roller fascial release
- Massage gun, 3x weekly since November 2022
- Radial Pressure Wave (RPW) 15 sessions, May-July 2023
- Weekly in StretchLab
All these treatments are standard protocols for “responsible pain management” in medical facilities. I have worked in a similar medical office for nearly two decades and observed first-hand the application and results of commonly accepted pain management. Chiropractors, physical therapists, and nurse practitioners designed treatment plans strictly on the location of the pain and other symptoms. For example, the initial diagnosis of this patient’s right hip pain and dysfunction was “elevation of the right hip.” No one tried to detect the initial trigger but instead treated her secondary symptoms.
Medical Massage Therapy
Before SOMI’s Medical Massage seminars and hands-on training, I worked on the patient using sessions of Therapeutic Massage with elements of Medical Massage focusing on areas of the patient’s complaints: Lumbar, Gluteal, Hamstring, and IT band. She felt some improvement but continued to suffer from the acute, bilateral burning pain in her hips and thighs.
During Ask-and-Show training with Dr. Ross, I brought up this case. We developed a new evaluation and treatment strategy to identify and eliminate the initial trigger rather than chasing the pain ghost.
Evaluation:
Detailed evaluation of the patient’s soft tissues in the lower back and hip area provided the following data:
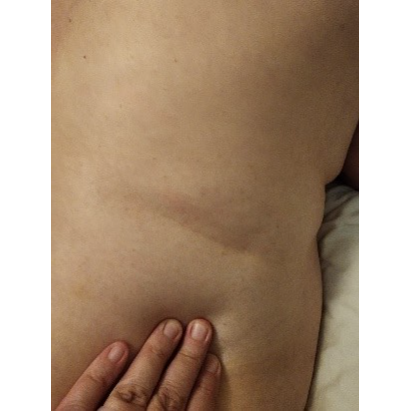
- Active connective tissue zones in the second (superficial fascia) and third (deep fascia) levels were detected in the lumbar area. However, the degree of fascial tension was far more significant on the right side, creating a visible crease that followed the last rib (see Fig. 1).
2. There were trigger points in the thoracic and lumbar erectors.
3. There were trigger points in the right Quadratus Lumborum Muscle. The upper TP below the 12th rib was especially active.
4. Even mild application of pressure during the Compression Test in front of the right sacroiliac joint immediately triggered referred pain to the gluteal area and thigh. Thus, the Compression Test confirmed irritation of the L5 spinal nerve between the last lumbar vertebra, sacrum, and right SI joint.
5. There were periosteal TPs along the last rib and the SI joint and sacrum
6. Examination of the patient’s thighs showed the presence of very significant fascial restrictions and muscle tension in the middle thigh, almost fist-sized on the right. It involved the vastus lateralis, biceps femoris muscle.
7. Both iliotibial bands showed significant fascial adhesions and restrictions of soft tissue mobility and elasticity, especially in the upper and middle thirds of both IT bands. The degree of tension was less in the lower third of the IT bands above the knee joints.
The first session of Medical Massage:
I started with the Medical Massage Protocol for the Lumbalgia concentrating only on lumbodorsal fascia and lumbar erectors. I separately worked on the skin within affected dermatomes, then on the superficial fascia, and finally on the lumbar erectors (insertions and muscle belly). I used superficial friction, skin rolling, the inhibitory regime of MT, engaged H-Reflex, Trigger Point Therapy, and finally Postisometric Muscle Relaxation.
By the end of the first session, the patient demonstrated an immediate decrease in pain intensity in the right lumbosacral region, and a Compression Test to examine the L5 spinal nerve in the area of the right SI joint was negative!
I gave her detailed instructions as homework to decrease tension in the Lumbar Erector and QL muscle. I also encouraged her to share my recommendations with her Stretchlab therapist to reinforce therapy during their weekly appointments additionally.
The second session of Medical Massage:
The patient reported a significant decrease in the intensity of pain and dysfunction in her lower back, after just the first session. To her complete surprise, she was able to do a lot of walking over the weekend without discomfort.
I used the same treatment strategy as the first session. The only addition was that I concentrated on the upper part of the lumbar erectors at the insertion to her 6th and 7th ribs. Initial improvement in the fascial tension in the CTZs on the right was retained since the first session.
I encouraged the patient to continue Lumbar and QL stretching at home and with the Stretchlab therapist during their weekly appointments.
The third session of Medical Massage:
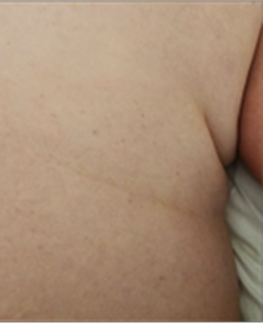
The patient reported a great overall improvement in pain intensity in the glutes, lateral hip, and IT bands. The burning pain had eased significantly; she felt it only if she was tired. Instead of acute pain, she described her symptoms as a mild ache. The skin crease below the last ribs on the right, which was the epicenter of her fascial tension was barely visible (see Fig. 2).
There are no clinical signs of tension in the CTZs on the right. Application of the Lateral Shift Technique on the left paravertebral indicated the presence of residual tension in the CTZs of the third level (there was restriction of the lumbar erectors’ lateral shift regarding the QL and iliopsoas muscles). The Compression Test continued to be negative. On her left side, the patient exhibited residual tension at the attachment of lumbar erectors (superior iliocostalis muscle).
Considering I had achieved almost complete functional restoration of the fascia and lumbar erectors, I switched my priority to the right QL muscle. I used the addition of Lumbalgia Protocol for the QL muscle. While I worked with even, moderate longitudinal and cross-fiber friction on the lateral edge of the right QL muscle, especially below the last rib, the patient reported acute pain.
We added Piriformis, Hamstring, Quad and IT band stretching at home and with the Stretchlab therapist.
Fourth Session of Medical Massage:
The patient reported “horrible” pain in the lateral and anterior hip that started after her last session and its intensity was still significant. Considering the patient’s reaction to my work on the right QL muscle at that time, a flare-up of pain and dysfunction was to be expected.
I used the same treatment as the previous session, but now I added elements of Tensor Fascia Latae Muscle Protocol on both sides and gave her the same homework.
I contacted the patient the next day after this session, and she reported that she could walk through a grocery store the same day without any pain.
Fifth Session of Medical Massage:
The patient reported a complete restoration of mobility. She started gym exercises with her personal trainer to build up lost muscle mass and restore normal reflex relations between muscle antagonists, which would reinforce soft tissue stability and prevent possible injuries or overload.
In this session, I addressed her thighs, especially the IT bands. I used the same protocol as the previous session but decreased my time working in the lumbar and gluteal areas, concentrating on the IT bands by applying different frictions, tissue displacement, and passive stretching. I encouraged her to concentrate on passive and assisted stretching of the thigh muscles and IT bands.
Sixth Session of Medical Massage:
The patient reported a complete disappearance of bilateral hip pain and burning sensations. She periodically felt an ache around her knees.
I applied bilateral application QL & TFL protocol, CTZ I & II to improve the lateral mid-thigh on both legs, CTZ for the positive right vastus intermedius, CTZ I & II for positive bilateral knees and anterior tibialis, and CTM for skin and superficial fascia.
I recommended the same homework be done regularly for two weeks with a gradual increase in exercise intensity in the gym. Currently, the patient is free of pain, and to let her system rest, I will see her every two weeks until all residual tension fades away.
MESSAGE FROM SOMI:
If therapists seek clinical training in Medical Massage theory and its application, consider joining SOMI for the live Webinars and Seminars in 2024. Here is a link to the following year’s schedule:
About the Author
Kristi Tidwell, LMT, CMMP has been practicing massage therapy for 21 years. Recently, she graduated from SOMI’s Medical Massage Certification Program and earned her CMMP Diploma.
‘I’ve been blessed to work alongside nurturing Chiropractors, Physical Therapists, Nurse Practitioners, Medical Doctors, and Osteopaths throughout my career. Each one taught me something new about medicine, pain management, and patient care. However, when I enrolled in the first Medical Massage Seminar presented by Dr. Ross Turchaninov in 2006, I was immediately amazed and enchanted by the Medical Massage course. I have extensively used the Medical Massage textbook in my practice for over 17 years. Over the years, I have always come back to SOMI for knowledge with intrigue and a growing understanding of chronic pain and its relationship with normal muscle and soft tissue function. I can confidently take all of these accumulated years of experience and truly produce therapy that is smart, effective, and efficient. Thank you, Dr. Ross and SOMI!!!’
Category: Case Studies
Tags: 2023 Issue #3