By Dr. Ross Turchaninov, MD
Let us start this important conversation with a very frequent clinical situation every therapist encounters practically daily. The patient comes to the clinic and complains about pain in the right upper shoulder which sometimes he feels in the neck and right shoulder joint. Pain increases with cervical, and shoulder joint ROM. Evaluation indicates the presence of acute pain when even the slightest pressure is applied (Jump Test is positive) in all areas associated with locations of active trigger points (TPs) in the right trapezius muscle. Thus, increased tension in the right trapezius muscle or Trapezius Muscle Syndrome (TMS) is obvious and it is also supported by postural changes: elevation of the right shoulder in combination with head extension due to additional increase of cervical lordosis.
We think that readers agree that this described situation is quite typical in our stress rich society. It seems that decrease of the tension in the trapezius muscle and elimination of active TPs are going to help this person. Thus, the therapist starts to work using techniques and modalities he or she was taught to use by an endless variety of seminars, textbooks, webinars etc. All these educational sources suggested to address tension in the trapezius muscle with this or that modality and the therapist follows required steps.
Now let us look at the same issue from the clinical approach to evaluation and application of massage therapy based on the science rather than personal opinions. There are no doubts that the patient has tension and active TPs in the trapezius muscle. No one disputes that obvious clinical finding. However, addressing the tension in the trapezius muscle itself, with all recommended modalities, is not a correct initial treatment strategy because the real cause for the TPs formation in the trapezius must be clearly established first.
What can cause active TPs formation in the trapezius muscle? There are five main causes and each of them is going to trigger the exact same clinical symptoms and only detailed evaluation allows identification of the real trigger and formulates the correct treatment strategy. Let’s discuss each of the main causes separately:
1. Trauma
There are no doubts that trauma (e.g. whiplash during car accident) is going to activate TPs creating the clinical picture of TMS. However, the patient must have had recent trauma to consider whether it is the cause of TMS. For example, the therapist must not think that the trauma is a cause of TMS symptoms if the accident happened two years ago. With such a long, chronic history other players (including the patient’s motor cortex) already stepped in and the therapist now is dealing with a much more complex, multilayered situation than just trauma of the trapezius muscle.
Fig. 1 illustrates our patient with left upper shoulder and neck pain due to an automobile accident that happened two weeks prior.
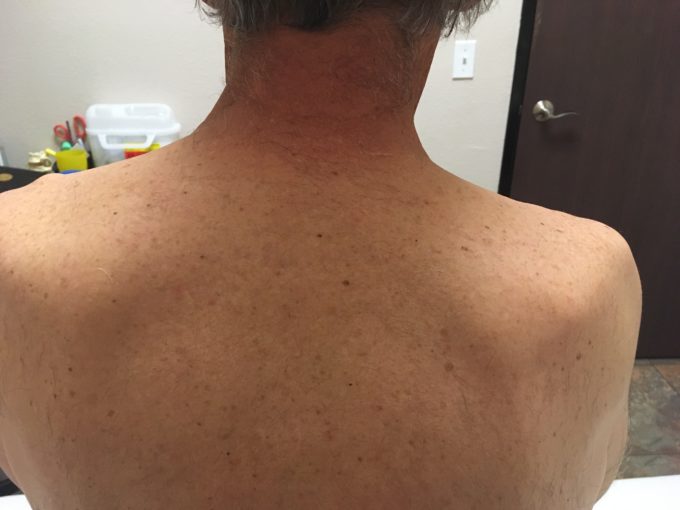
Fig. 1. The left TMS due to the auto accident
As readers can see, the visual change is elevation of the left shoulder due to the protective spasm of injured trapezius muscle, outer rotation (visual bulging) of the left scapula compared to the right one (the patient is right handed) due to the strain of left levator scapulae muscle. Also, the patient exhibited active TPs in posterior cervical muscles in the middle and deep layers. An MRI conducted after the accident did not record any trauma to the vertebrae and no significant deterioration of the cervical disks. Other clinical tests were negative as well. Thus, the obvious cause of the TMS is whiplash trauma.
2. Postural Overload
Yes, incorrect ergonomics in our computers and cellular phone society can contribute to the TMS. However, the therapist may consider the postural overload as a trigger, only if rest of causes we are discussing below are ruled out.
Fig. 2 illustrates tension in the left trapezius muscle due to incorrect distribution of the vertical load caused by wrong ergonomic.
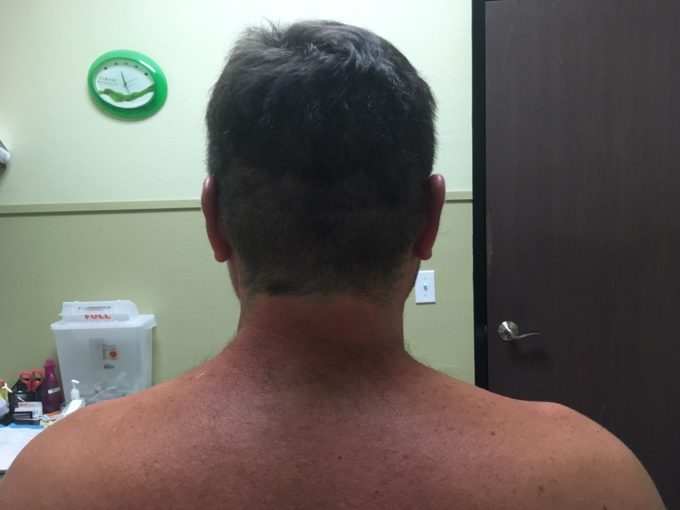
Fig. 2. Left side TMS due to incorrect ergonomic
The patient is a computer programmer who works for hours on a computer while holding his elbows in the air and sitting on the edge of the chair. Such incorrect posture in combination with a lot of isometric work by trapezius triggered acute pain in the left shoulder. All other clinical tests were negative. The readers may again observe milder elevation of the left shoulder and active TPs were present in upper and lower parts of trapezius muscles, especially on the left. The patient also exhibited tension in the levator scapulae muscle which readers can see as tissues’ puffiness above upper medical angle of the left scapula.
3. Intervertebral Disk Pathology And/Or Tension In The Posterior Cervical Muscles
The trapezius muscle is innervated from two sources: assessory nerve and C2-C4 spinal nerves.
If, even early stages of disk degeneration formed on the level C2-C4 or tension in the middle or deep layer of posterior cervical muscles (e.g. semispinalis capitis muscle) developed the first clinical symptoms the therapist is going to see is formation of TMS. In this scenario TMS is reflex reaction to the initial trigger which is disk pathology or/and posterior cervical muscles tension, which is always present in cases of disk degeneration.
Fig. 3 illustrates our patient with left side neck and cervical pain while the real cause was disk herniation on the level C4-C5 confirmed by cervical MRI. At the moment this picture was taken, her only complaints were acute pain in the left upper shoulder. TPs in the same locations were detected. As you can see, the patient’s left shoulder is again visually elevated, tissues in left anterior neck are thicker compared to the right side (the patient is right handed) and she tilts her head to the right. The last symptom is brain’s protective reflex reaction. By tilting the head to the right brain increases space between two vertebrae and open spinal foramen. That is protective reaction brain uses to decompress spinal cord and C4-C5 spinal nerves already compromised by the degenerated disk.
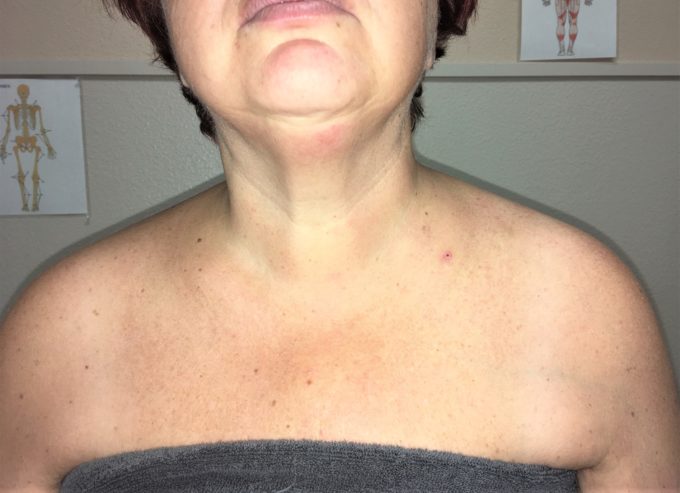
Thus, based on this patient’s symptoms, it is impossible to differentiate if the cause of TMS is postural overload or small bulge of C4. Reaction of the trapezius muscle is going to be exactly the same!
4. Tension In The Upper Portion Of The Anterior Scalene Muscle (ASM)
Tension in the ASM, especially in its upper third, is going to trigger TMS as an initial reflex reaction. Again, the clinical symptoms of TMS are going to be identical to postural overload or to disk degeneration of posterior cervical muscles’ tension with the exact same location of active TPs and ROM deficiency. That happens because C2-C4 spinal nerves which innervate ASM are also contribute to the cervical and brachial plexuses which are responsible for the innervation of tissue in the upper body and extremities. Even mild tension in ASM may irritate cervical and/or brachial plexuses where C2-C4 nerves are and it triggers clinical picture of TMS as a reflex reaction to ASM’s tension.
Fig. 4 illustrates our patient with severe spasm in the left trapezius muscle with multiple TPs locations and severe ROM restriction due to compression of the upper brachial plexus by tensed ASM.
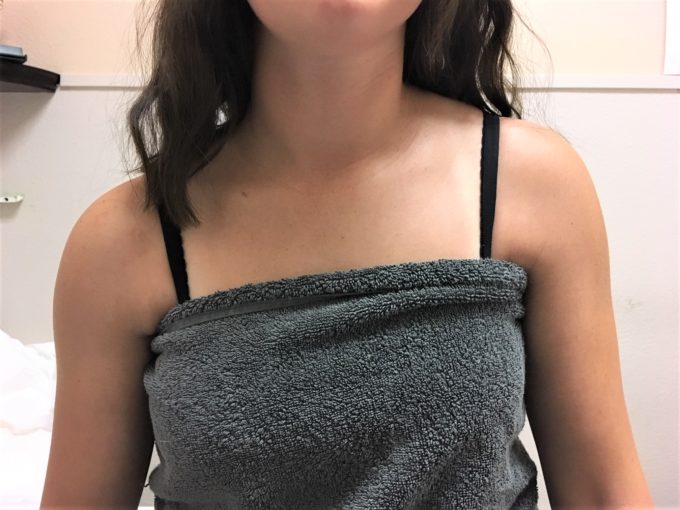
Fig. 4. Left TMS due to the significant tension in the left anterior scalene muscle (ASM)
This patient with TMS, which was originally triggered by tension in the ASM, besides pain in the left neck and upper shoulder suffered from severe migraine-type headache from the occipital part of the head all way to the left eye (cluster headache). She also recently noticed ‘pins and needs’ sensations (paresthesia) formed around her left thumb which is additional indicator of upper brachial plexus’s compression which now contributes to radial nerve’s inflammation (Radial Nerve Neuralgia). Thus, the irritation of the brachial plexus by tensed left ASM caused spasm in the left trapezius muscle and it is pure reflex reaction. This reaction is clearly visible as higher elevation of the left shoulder and body does that to decompress brachial plexus and protect it from further damage. Also very tensed trapezius or more precisely upper part of the its vertical portion compressed greater occipital nerve triggering Cluster Headache. This is perfect example of multilayered pathology formed in the upper body due to the simple thing – tension in the ASM.
Our attempt to examine ASM using Wartenberg’s Test triggered severe pain and withdrawal reaction, which pain radiated all the way back to the patient’s left scapula and appearance of numbness around her left thumb. With other tests negative, positive Wartenberg’s Test was indicator of tensed ASM being the initial trigger of TMS.
5. Chronic Pulmonary or Hepatic abnormalities
If the patient suffers from chronic pulmonary or hepatic (i.e., liver) abnormalities the therapist may observe a clinical picture of TMS similar to postural overload or trauma, but in this case it is reflex or somatic reactions to the presence of chronic visceral pathology (in lungs or liver). These reflex abnormalities in the function of soft tissues are mediated by viscera-somatic and viscera-motor reflexes which are responsible for the formation of reflex abnormalities in the soft tissues including active TPs in the trapezius muscle due to the initial presence of chronic visceral disorder(s).
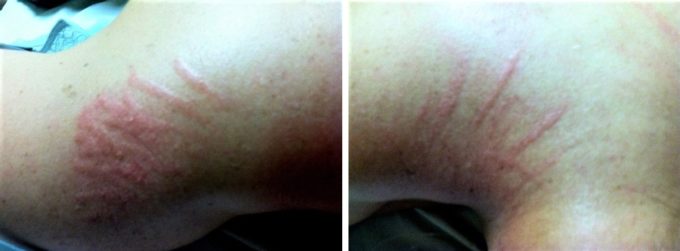
Fig. 5. Excessive Red Dermographism reaction of the skin over the right shoulder and neck in patient after right side pneumonia.
This skin reaction happened seeing in the picture is from simple distribution of oil (same oil was used on this patient before for different reasons). The patient came with acute pain in the right upper neck and shoulder which started after she was discharged from the hospital finishing 10 days intense treatment of severe right-side pneumonia. Besides acute spasm in the right trapezius muscle the patient exhibited reflex zones formation in all layers of the soft tissues from the skin to the fascia, muscles and periosteum.
Reaction of the skin in the form of Excessive Red Dermographism is a 100% indicator of cutaneous reflex zones formed as somatic reaction to pneumonia.
So, we identified 5 most frequent causes of the TMS. What united all of them was the exact same clinical picture starting with patients’ complaints all way to the visual and palpatory evaluation. The only difference in each picture is the degree of spasm in the trapezius which defines the intensity of the symptoms, degree of shoulder’s elevation and ROM restriction.
Thus, to deliver stable clinical results the therapists must determine the initial trigger of TMS since each cause of TMS requires its own separate treatment strategy. Technically speaking therapist faces five different ways of treating look like exactly the same symptoms of TMS.
Let’s discuss same causes, but now from the treatment point of view:
1. Trauma
This client/patient indeed requires local therapy in the form of Trigger Point Therapy, Myofascial Release, Muscle Energy Techniques etc. In this case the therapy should be exactly as it was suggested to the therapists by their instructor or textbook on how to address tension in the trapezius muscle.
2. Postural Overload
For this client/patient the same treatment strategy as local therapy should be implemented. However, the ergonomic correction and later addition of the kinesiology-based techniques is the correct treatment strategy.
3. Intervertebral Disk Pathology And/Or Tension In The Posterior Cervical Muscles
If evaluation confirms that one or both of these causes involved the therapist doesn’t have professional rights (of course if therapist really concerns about the patient) to apply local therapy only as mentioned in case of trauma or postural overload. Yes, local therapy is going to make the client/patient feel less pain, or even diminish pain and dysfunction to the acceptable levels, but such partial treatment is going to have only a temporary impact and the same tension is going to come back eventually.
For this group of patients, the MM protocol for Cervicalgia must be used first to decompress affected cervical disk(s) and/or decrease tension in the posterior cervical muscles. Later, the local therapy for TMS must be added to eliminate secondary symptoms in the form of active TPs. Of course, other modalities targeting degeneration of intervertebral disk or tension in the posterior cervical muscles can be used as well. The advantage of MM protocol is the simple fact that it combines clinically tested modalities together instead of their singular application.
4. Tension In The Upper Portion Of The Anterior Scalene Muscle (ASM)
If during evaluation the therapist gets a clear reading that Wartenberg’s Test is positive and tension in ASM is present, the therapist again does not have professional rights to apply local therapy to address tension in the right trapezius muscle as the main treatment goal. The MM protocol to address tension in ASM must be used first and after Wartenbegr’s Test becomes negative the local therapy in the trapezius muscle must be conducted.
5. Chronic Pulmonary or Hepatic Abnormalities
For these patients the local therapy becomes priority since tension in the trapezius muscle is secondary or reflex reaction of the soft tissues to the chronic pulmonary of hepatic abnormalities. However, for these patients the addressing only trapezius’s hypertonicity in form of active TPs is not enough. If reflex zones are formed in the soft tissues because of chronic visceral disorder the pathological changes are going to affect all four types of the soft tissues (skin, fascia, muscle, periosteum). Thus, the therapist must pay attention to individual changes in each type of the soft tissues and address them separately with specific treatment methods or techniques.
For example, the patient with chronic inflammation in the gall bladder (i.e., cholecystitis) secondarily developed TMS. For this patient any type of clinical bodywork targeting trapezius muscle itself is going to bring only temporary relief because the ultimate solution to the pain and dysfunction in the right upper shoulder and neck is normalization of gall bladder function or its removal.
Thus, in cases of intervertebral disk pathology and/or tension in the posterior cervical muscles; tension in the Anterior Scalene Muscle; Chronic Pulmonary or Hepatic disorders presence of the active TPs in the right trapezius muscle are a classic examples of reflex zones formation.
Here is a legitimate question: Why one of the first symptoms of disk degeneration, tension in the posterior cervical muscles, tension in the ASM or chronic visceral pathologies is TMS? The answer to this question is a complex chain of events which is responsible for the formation of secondarily reflex zones in the soft tissues including skeletal muscles. From one side they are cause of the clinical symptoms which brought client/patient to the clinic, but from the other side they are not the original trigger, but rather a neurological reaction to it, since even mild irritation of motor cortex or/and peripheral NS are directly responsible for reflex zones formation. The very confusing factor is that the initial trigger can be in a completely different part of the body and in early stages it shows itself in the form of reflex zones only (active TPs in trapezius m.). At that time, the patient very rarely complains about any discomfort or any clinical symptoms in the initial trigger’s location. Thus, the correctly and meticulously conducted evaluation of each potential cause is only the foundation to get the stable clinical results. Such strategy gives the therapist the opportunity to knock on the correct treatment door from the very beginning.
If the patient has symptoms of TMS as the result of reflex zones formation and the therapist uses local therapy as the main treatment tool, as frequently recommended by a majority of educational sources, there is no way stable clinical results can be achieved in 100% of cases. In our clinic we observe a lot of patients with TMS and only a minority of them have trauma or postural overload as the initial trigger. In a majority of cases the other three causes are more prevalent and local therapy eventually becomes a wasting of the patient’s money and the therapist’s time.
The mechanism of reflex zones formation all with necessary references we will discuss separately in Part II and Part III of this article.
Category: Medical Massage
Tags: 2020 Issue #2
