MEDICAL MASSAGE VS MIGRAINE TYPE CLUSTER HEADACHE
by Dr. Ross Turchaninov
My thanks to everyone for posting your comments. Let’s first address some concerns therapists expressed in their posts. Clinical reasoning includes three equally important components: Visual Observation, Clinical Interview and Palpatory and Function Examination. We published detailed articles on these subjects in the previous issues of JMS. For those who are curious here are links:
1. Science of Visual Evaluation:
Science of Massage Institute » The Science of Visual Evaluation
2. Science of Clinical Interview:
Science of Massage Institute » SCIENCE OF CLINICAL INTERVIEW
3. Science of Palpation:
Science of Massage Institute » Science of Palpation Part I
Science of Massage Institute » THE SCIENCE OF PALPATION PART II. SKIN AND CONNECTIVE TISSUE ZONES
Science of Massage Institute » PALPATION OF THE SOFT TISSUE IN THE MIDDLE LAYERS
Science of Massage Institute » THE SCIENCE OF PALPATION. PART IV DEEP PALPATION OF THE SOFT TISSUES
Information we shared in this and previous posts on Clinical Reasoning covers ONLY visual observation which must be followed by an interview and clinical examination. The visual observation is first and sometimes the important step which initially sends the therapist’s thoughts in the correct direction. Thus, the entire evaluation starts not at the moment of patient/client information’s intake but at the moment of the first visual contact. Thus, our goal is to train the therapists’ eyes to the correct interpretation of visible changes the patient/client’s body exhibits during the first visual contact. Interview, palpatory examination are next steps in the evaluation.
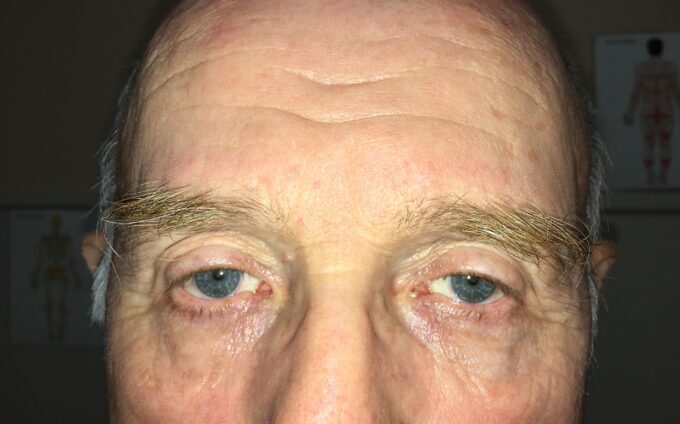
Initial question was: Taking a first look at the patient’s face indicates two possible causes for visiting the clinic. What are those two pathological conditions?
The condition you observe on the photo is called Ptosis or drop of the upper lid. Some therapists correctly identified the two most frequent causes of the Ptosis: face paralysis (Bells’ Palsy, Myasthenia Gravis, etc.) and Headache. This patient was referred to our clinic by a neurologist and he suffered with the typical clinical picture of Migraine Type Cluster Headache.
That brings us to ‘I can’t diagnose’ comments which were frequently posted. Our patient already arrived with a diagnosis of Chronic Headache which was very difficult to control even with medications. Visual observation as well as further interview and palpatory evaluation indicated classic case of Cluster Headache rather than general term of Chronic Headache. That is a very important distinction from the treatment perspective since the patient with Chronic Headache and Chronic Cluster Headache have different treatment strategies as you will see later in the treatment section. Thus, you are not diagnosing but rather fine tuning your treatment strategy based on the collected data including the visual observation.
If you see a patient in your clinic who looks very tired, moves slowly has one side Ptosis especially with lacrimation you may suspect a case of Cluster Headache or Cluster Migraine. The presence or absence of previous Bell’s Palsy or Myasthenia Gravis could be ruled out during further intake and examination. Our patient did not exhibit any weakness of the facial musculature and there was no Myasthenia Gravis in his history.
The major complaint from patients with Cluster Headache is a debilitating headache which can affect the entire half of the head and centered behind eyeball or concentrated only behind the eyeball. It may be accompanied by excessive lacrimation, light phobia, nausea, and even vomiting. If you enlarge the picture you may notice more tears formed above the lower lid of the left eye and the upper lid is very swollen. Frequently powerful medications don’t even touch the pain intensity of Cluster Headache and patients run to the ER for IV application.
Soft tissues in the orbit including the eye muscles are innervated by the trigeminal nerve which originates from the brain itself and is called cranial nerve. One of the major causes of Cluster Headaches is compression of the greater occipital nerve (which is the spinal nerve) by tensed posterior cervical muscles. Chronic irritation of the greater occipital nerve trigger relatively recently discovered clinical phenomenon called Occipital-Trigeminal Convergence. In this case the irritation and inflammation of the greater occipital nerve on the back of the head causes the reflex hyperirritability of the trigeminal nerve which is responsible for sensory innervation of the face and motor innervation of eye muscles. Occipital-Trigeminal Convergence reflex works in the opposite direction as well. That’s why patients with Trigeminal Neuralgia frequently exhibit Occipital Headaches.
Tension of the tissues in the orbit especially Tenon’s Capsule and spasm of eye muscles trigger the eyeball’s protrusion from the orbit. This protrusion elicits great pressure on the optic nerve which connects the eyeball to the visual cortex. Overstretching of the optic nerve is the immediate cause of a Cluster Headache located behind the eye, however, the initial trigger of a Cluster Headache is still tension in the posterior cervical muscles and compression of the greater occipital nerve at their insertion into the occipital ridge.
The cause of the ptosis in the patient with Cluster Headache is a brain protective reaction. By dropping the upper lid, the brain decreases the amount of light entering the eye and it diminishes the working pressure on an already inflamed optic nerve.
Of course not all patients with Cluster Headache exhibit Ptosis but if it is present it means long, chronic history of disorder.
HISTORY
Our patient suffered with CH for several years. It started on the back on his head but recently concentrated around the eye. Prescribed medications were not able to control the pain intensity. In this case his original Tension Headache was slowly transformed into Migraine-Type Cluster Headache. He didn’t have True Migraine because he didn’t have aura before attack.
EVALUATION
Even mild application of the Compression Test at the insertion of the posterior cervical muscles into the occipital ridge triggered a very intense headache around the left eye. All four Grinstein’s Points associated with severe shortening of cranial aponeurosis were positive especially on the left. The left eye ball was protruding from the orbit compared to the right one. Even mild application of the pressure around the orbit worsens the headache. The Sensory Test indicated sensory deficit on the left forehead due to hyperirritability of the supraorbital division of the trigeminal nerve. Of course there was wide spread tension in all layers of the posterior and anterior neck muscles.
To summarize logical chain of events: chronic tension in the posterior cervical muscles – irritation of the greater occipital nerve – occipital headache – triggering of occipital-trigeminal convergence reflex – hyperirritability of the trigeminal nerve – increased tension within the soft tissue of the orbit including ocular musculature – stretching of optic nerve -Migraine-type Cluster Headache.
THERAPY
The Medical Massage treatment strategy consisted of decompression of the greater occipital nerve by resetting posterior cervical muscles and fascia, stretching of cranial aponeurosis and eye therapy to re-position eyeball in the orbit to take pressure from the overstretched optic nerve. As the patient was completely rehabilitated he slowly eliminated all pain medications.
If case of Cluster Headache wasn’t specified during evaluation and headache was only treatment target, without decompression of the soft tissues in the orbit, there is great chance that symptoms are going to return.
This is very short overview of very complex topic. If you would like to learn all aspects of rehabilitation of Headaches including Cluster Headaches to decisively help these patients, we are going to refer you to the 5 part article (with all necessary references) on the pathology and Medical Massage treatment of Headaches including Cluster Headache published in previous issues of JMS.
Part I:
Part II:
Part III:
Part IV:
Part V:
SOMI was invited to train therapists at Barrow Neurological Institute, a world leading scientific neurology institution, on this topic. The Medical Massage protocol presented in the links above is currently used there as a routine medical procedure to rehabilitate patients with Tension Headache, Migraine-type Headaches and True Migraines.
Category: Blog